Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Learn about pneumococcal meningitis, a serious bacterial infection of the brain and spinal cord membranes. Understand its causes, rapid symptoms, diagnosis, treatment, and crucial prevention methods including vaccination.

What is Pneumococcal Meningitis? Pneumococcal meningitis is a serious and potentially life-threatening infection that affects the membranes surrounding the brain and spinal cord. These protective membranes are known as the meninges. The culprit behind this specific type of meningitis is the Streptococcus pneumoniae bacteria, a common bacterium that many people carry in their nose or throat without experiencing any illness. However, when this bacteria manages to invade the bloodstream and travel to the meninges, it can trigger a dangerous inflammation. It's important to understand that while many people are carriers of Streptococcus pneumoniae , the bacteria remain dormant in the vast majority of cases. This means they are not actively multiplying or causing harm. But, under certain circumstances, these dormant bacteria can become active and lead to severe infections. Even with prompt medical attention and treatment, pneumococcal meningitis carries a significant risk, with up to 20% of those affected succumbing to the illness. Furthermore, a substantial number of survivors, around 20%, may face long-term health complications. Meningitis, in general, is characterized by the inflammation of the meninges. While viral infections are the most common cause of meningitis, pneumococcal meningitis is specifically a bacterial form. Its severity cannot be overstated, as it poses a grave threat to life, even when managed by medical professionals. Symptoms of Pneumococcal Meningitis The onset of symptoms for pneumococcal meningitis can be quite rapid, often appearing one to three days after exposure to the bacteria. However, in some instances, the timeline might be shorter or longer. Recognizing these symptoms promptly is crucial for seeking immediate medical help. Common symptoms include: Sudden high fever Severe headache Stiff neck Nausea and vomiting Sensitivity to light (photophobia) Confusion or difficulty concentrating Seizures In infants, the signs might be less specific and can include: Irritability and crying Excessive sleepiness or difficulty waking up Poor feeding A bulging soft spot (fontanel) on the head Other potential symptoms that may arise include a rash, particularly in some types of bacterial meningitis, and a general feeling of being unwell. Causes and Transmission Pneumococcal meningitis occurs when the Streptococcus pneumoniae bacteria enter the bloodstream, breach the blood-brain barrier, and begin to multiply in the cerebrospinal fluid (CSF) that surrounds the brain and spinal cord. This fluid is vital for cushioning and protecting these central nervous system components. While Streptococcus pneumoniae is the direct cause of pneumococcal meningitis, these bacteria are also responsible for other common infections, such as: Pneumonia (lung infection) Bacteremia (blood infection) Sinusitis (sinus infection) Otitis media (ear infection) Transmission of the bacteria typically happens through respiratory droplets expelled when an infected person coughs or sneezes. Close contact, such as kissing or sharing items that come into contact with the mouth (like utensils, cups, or even cigarettes), can also facilitate the spread of the bacteria. Living in close quarters with many people, such as in dormitories or military barracks, can increase the risk of transmission due to the higher likelihood of close contact. Diagnosis Diagnosing pneumococcal meningitis usually involves a combination of clinical evaluation and laboratory tests. The cornerstone of diagnosis is often a lumbar puncture , also known as a spinal tap. During this procedure, a healthcare professional carefully collects a sample of cerebrospinal fluid from the lower back. Analysis of the CSF sample is critical. It allows doctors to: Identify the presence of bacteria, specifically Streptococcus pneumoniae . Determine the type and number of white blood cells, which indicate inflammation. Check for other markers of infection. In addition to the spinal tap, a thorough physical examination is performed. Doctors will look for specific signs and symptoms suggestive of meningitis, such as a stiff neck, fever, and altered mental status. Blood tests may also be conducted to check for signs of infection in the bloodstream and to identify the bacteria. Treatment Options Pneumococcal meningitis is a medical emergency requiring immediate treatment. The primary treatment involves the administration of antibiotics . The choice of antibiotic and the duration of treatment will depend on the severity of the infection, the specific strain of bacteria, and the patient's overall health. Intravenous (IV) antibiotics are typically given in a hospital setting to ensure rapid delivery and high concentrations of the medication reach the brain and spinal cord. In some cases, corticosteroids may also be prescribed to help reduce inflammation in the meninges, potentially lessening the risk of long-term complications. Supportive care is also a vital part of treatment. This may include: Intravenous fluids to prevent dehydration Medications to manage fever and pain Monitoring for and managing seizures Respiratory support if needed It is crucial to complete the full course of antibiotics as prescribed by the doctor, even if symptoms improve, to ensure the infection is completely eradicated. Prevention Strategies Preventing pneumococcal meningitis is paramount, and vaccination plays a key role. There are vaccines available that offer protection against various types of Streptococcus pneumoniae bacteria. The pneumococcal vaccines are generally recommended for: Infants and young children (as part of routine immunization schedules) Adults aged 65 years and older Individuals with certain chronic health conditions (such as heart disease, lung disease, diabetes, or weakened immune systems) Smokers Individuals with asthma Besides vaccination, good hygiene practices can also help reduce the risk of transmission: Frequent handwashing with soap and water Covering the mouth and nose when coughing or sneezing Avoiding close contact with sick individuals Not sharing personal items like cups, utensils, or toothbrushes When to Consult a
In summary, timely diagnosis, evidence-based treatment, and prevention-focused care improve long-term health outcomes.
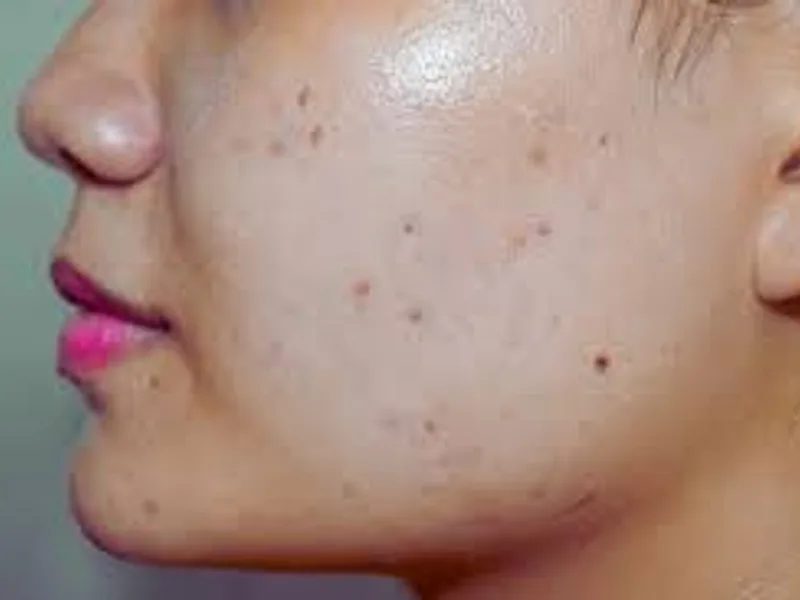
Discover proven methods to remove dark spots on your face. Learn about causes, treatments, and prevention from medical experts.
April 23, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.
April 20, 2026

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026