Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.

Malaria, a serious and sometimes fatal illness, is caused by Plasmodium parasites transmitted through the bite of infected mosquitoes. Early and accurate diagnosis is absolutely crucial for effective treatment and preventing severe complications.
Among the diagnostic tools available, the peripheral blood smear remains a cornerstone, offering direct visualization of the malaria parasites within a person's blood.
Practically speaking, when malaria is suspected, physicians often order a peripheral blood smear. This test involves examining a small drop of blood under a microscope.
It’s a time-tested method that allows specialists to identify not only the presence of the parasite but also the specific species and the level of infection. This information is vital for guiding appropriate therapy.
A peripheral blood smear is a diagnostic procedure where a thin layer of blood is spread onto a glass slide, stained, and then examined under a high-powered microscope. This technique allows for the evaluation of various blood components, including red blood cells, white blood cells, and platelets.
For malaria diagnosis, the focus is on detecting the presence of Plasmodium parasites within the red blood cells.
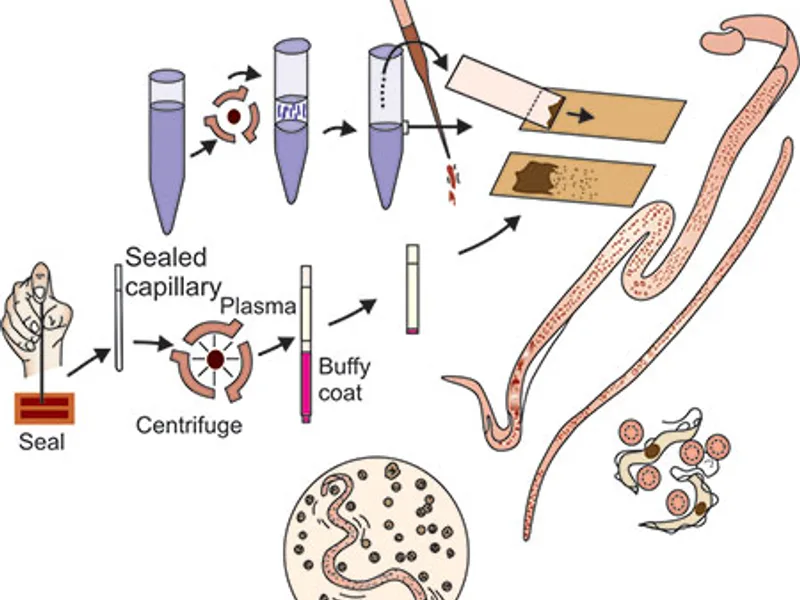
Obtaining a peripheral blood smear is a relatively straightforward process. First, a healthcare professional will clean a small area of your skin, usually on your fingertip or arm, with an antiseptic. Then, using a sterile lancet, they will prick the skin to obtain a small blood sample. This blood is then carefully spread onto a clean glass slide.
Here's where it gets interesting.
Two types of smears are typically prepared: a thin smear and a thick smear. The thin smear involves spreading a single layer of blood cells, which helps in identifying the species of the Plasmodium parasite and assessing the morphology of infected cells.
In contrast, the thick smear uses a larger volume of blood, concentrated by lysing (breaking open) the red blood cells. This concentration significantly increases the chances of detecting parasites, especially in cases of low-grade parasitemia (low parasite count).
After preparation, the slides are stained, most commonly with Giemsa or Wright's stain. These stains highlight the parasites, making them visible against the background of blood cells. A trained microscopist then meticulously examines the stained smear under a microscope, looking for characteristic parasites.
When examining the blood smear, physicians and laboratory technologists are searching for specific indicators of malaria. These include the presence of ring forms, trophozoites, schizonts, and gametocytes of the Plasmodium parasite within the red blood cells (for thin smears) or free in the blood (for thick smears).
It sounds simple. It rarely is.
Different Plasmodium species—such as *Plasmodium falciparum*, *Plasmodium vivax*, *Plasmodium ovale*, and *Plasmodium malariae*—have distinct appearances and life cycle stages that can be identified under the microscope. Does this sound familiar?
The morphology of the infected red blood cells also provides clues. For instance, *P. vivax* and *P. ovale* can cause infected red blood cells to enlarge, a sign not typically seen with *P. falciparum* or *P.
malariae*. Quantifying the level of parasitemia is another vital aspect. This is usually expressed as the percentage of infected red blood cells or the number of parasites per microliter of blood. Higher parasite counts often correlate with more severe disease, particularly with *P. falciparum* infections.
A positive result on a peripheral blood smear indicates the presence of malaria parasites, confirming the diagnosis. The report will usually specify the Plasmodium species identified and the level of parasitemia.
The numbers don't lie.
A negative result, however, does not always rule out malaria, especially if the blood was drawn during an early stage of infection or if the parasite count is very low. In such instances, repeat testing or alternative diagnostic methods might be recommended.
Honestly, interpreting these results requires significant expertise. The presence of specific parasite stages and the overall parasite load are key factors that influence the physician’s care strategy.
For example, *P. falciparum* infections, especially those with high parasitemia, require prompt and aggressive care due to their potential for rapid progression to severe malaria.
The peripheral blood smear is considered the gold standard for malaria diagnosis in many settings for several compelling reasons. Firstly, it is a relatively inexpensive test, making it accessible even in resource-limited areas where malaria is most prevalent.
Secondly, it does not require sophisticated equipment, just a microscope and trained personnel. Thirdly, it can accurately identify the infecting Plasmodium species, which is crucial as different species require different therapy approaches.
The numbers don't lie.
On top of that,, the test can provide information about the parasite density, helping clinicians gauge the severity of the infection and monitor the response to therapy. This direct visualization capability is something that some other diagnostic methods lack.
Despite its strengths, the peripheral blood smear has limitations. Its accuracy is highly dependent on the skill of the microscopist.
In real-world terms, if the person reading the slides is inexperienced, false negatives (missing an infection) or false positives (incorrectly identifying an infection) can occur. Additionally, preparing and examining smears can be time-consuming, and results may not be available as quickly as with some other tests.
For these reasons, other diagnostic tools have been developed and are used alongside or as alternatives to the blood smear. These include rapid diagnostic tests (RDTs), which detect parasite antigens in the blood, and molecular methods like polymerase chain reaction (PCR), which are highly sensitive and can detect very low levels of parasite DNA. So what does that mean for you?
While RDTs offer speed and ease of use, they may not always identify the species or quantify parasitemia as accurately as a smear. PCR is very accurate but is more expensive and requires specialized laboratory facilities.
Recovery is rarely linear.
The peripheral blood smear is not just for initial diagnosis; it also plays a vital role in monitoring the effectiveness of malaria therapy. Regular blood smears can be performed during the course of therapy to check if the parasite count is decreasing.
A sustained absence of parasites in the blood indicates that the therapy is working and the infection is being cleared.
This ongoing assessment helps physicians adjust the therapy plan if necessary, ensuring that patients receive the most impactful care. Enhancing patient outcomes relies heavily on this vigilant monitoring.
The peripheral blood smear remains a vital and reliable method for diagnosing malaria. Its ability to directly visualize and identify malaria parasites and their species, coupled with its cost-effectiveness and accessibility, ensures its continued importance in the global fight against this disease.
While newer technologies offer alternatives, the expertise gained from mastering the blood smear technique continues to assist physicians in providing optimal care for those affected by malaria.

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and why it's a vital tool in combating this disease.
April 20, 2026
Understand the wet mount parasite test: what it is, why it's done, and how it helps diagnose infections for better health outcomes.
April 20, 2026