Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Learn about MRSA, an antibiotic-resistant staph bacteria. Understand its types (HA-MRSA and CA-MRSA), causes, symptoms, risk factors, diagnosis, treatment, and prevention strategies.

What is MRSA? Methicillin-resistant Staphylococcus aureus (MRSA) is a type of bacteria that has developed resistance to certain antibiotics, specifically methicillin and other beta-lactam antibiotics. Staphylococcus aureus , often called 'staph,' is a common bacteria that lives on the skin and in the nose of many healthy people, usually without causing any problems. However, when staph bacteria enter the body through a cut or wound, they can cause infections. MRSA is a particularly concerning strain of staph because it is harder to treat with standard antibiotics. According to the Centers for Disease Control and Prevention (CDC), approximately one-third of all people carry Staphylococcus aureus bacteria, but only a small percentage of these individuals carry the MRSA strain. It's estimated that about 2 out of every 100 people carry MRSA. While MRSA can be found in both community settings and healthcare facilities, it is significantly more prevalent and poses a greater risk in hospitals and other healthcare environments. Types of MRSA There are two main types of MRSA infections: 1. Healthcare-Associated MRSA (HA-MRSA) This is the most common type of MRSA infection. HA-MRSA typically spreads among patients in hospitals, nursing homes, and other healthcare settings. Individuals who have weakened immune systems, invasive medical devices like catheters or IV lines, or recent surgery are at higher risk of contracting HA-MRSA. These infections can be serious and require prompt medical attention. 2. Community-Associated MRSA (CA-MRSA) CA-MRSA infections occur in people who have not recently been in a healthcare facility. This type of MRSA often spreads through direct skin-to-skin contact, especially when there are open cuts or scrapes. CA-MRSA is commonly seen in settings where people are in close contact, such as: Sports teams Dormitories Correctional facilities Military training centers Homeless shelters CA-MRSA often starts as a skin infection, appearing as a small bump or boil that may be red, swollen, and painful. It can sometimes resemble a spider bite. Causes of MRSA The development of antibiotic resistance in bacteria like MRSA is a complex issue primarily driven by the overuse and misuse of antibiotics over several decades. When antibiotics are used, they kill susceptible bacteria, but any bacteria that possess resistance traits can survive and multiply. This process, known as natural selection, leads to the proliferation of antibiotic-resistant strains. The more antibiotics are used, especially unnecessarily or incorrectly, the more opportunities bacteria have to evolve and develop resistance. This is why it's crucial to only take antibiotics when prescribed by a doctor and to complete the full course of treatment, even if you start feeling better. Risk Factors for MRSA The risk factors for developing MRSA differ depending on whether it's HA-MRSA or CA-MRSA: Risk Factors for HA-MRSA: Being in a hospital or healthcare facility for a long time. Having invasive medical devices, such as catheters, feeding tubes, or IV lines. Having a weakened immune system due to illness or medical treatment. Undergoing surgery or having wounds or surgical sites. Previous exposure to antibiotics. Risk Factors for CA-MRSA: Close skin-to-skin contact with someone who has an MRSA infection. Living in crowded conditions. Sharing personal items like towels or razors. Participating in contact sports. Having open cuts, scrapes, or other skin injuries. Injecting drugs, especially with non-sterile needles. Engaging in sexual activity without barrier protection. Symptoms of MRSA MRSA infections often begin as skin infections. The symptoms can vary depending on the location and severity of the infection, but common signs include: A red, swollen, and painful lump or boil on the skin. The lump may be warm to the touch. It may contain pus and can be mistaken for a spider bite. Fever. If MRSA enters the bloodstream or affects internal organs, symptoms can be more severe and may include: High fever and chills. Severe pain and swelling. Shortness of breath. Chest pain. Headache. Rash. Fatigue. Diagnosis of MRSA Diagnosing MRSA typically involves a laboratory test. A healthcare provider will take a sample from the infected area, such as a swab from a skin lesion, a blood sample, or a urine sample. This sample is then sent to a laboratory to identify the presence of Staphylococcus aureus and to determine its susceptibility to various antibiotics. This testing is crucial to confirm if the infection is indeed MRSA and to guide the selection of the most effective treatment. Treatment for MRSA Treatment for MRSA depends on the type and severity of the infection. For mild skin infections, topical antibiotics or drainage of the abscess might be sufficient. However, for more serious or invasive MRSA infections, stronger antibiotics are required. Since MRSA is resistant to many common antibiotics, doctors will prescribe specific medications that are effective against this strain. In some cases, surgery may be necessary to drain large boils or infected areas. It is vital to complete the entire course of prescribed antibiotics, even if symptoms improve, to ensure the infection is fully eradicated and to prevent the development of further resistance. Prevention of MRSA Preventing the spread of MRSA involves good hygiene practices and specific measures in healthcare settings: General Prevention Tips: Practice good hand hygiene: Wash your hands frequently with soap and water for at least 20 seconds, or use an alcohol-based hand sanitizer if soap and water are not available. Keep cuts and scrapes clean and covered: Wash wounds thoroughly and cover them with a clean bandage. Change bandages regularly. Avoid sharing personal items: Do not share towels, razors, clothing, or
In summary, timely diagnosis, evidence-based treatment, and prevention-focused care improve long-term health outcomes.
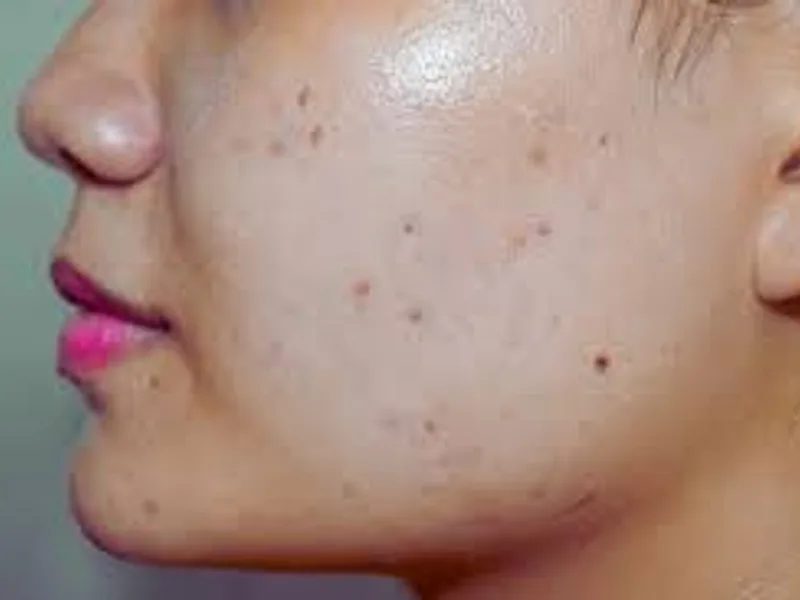
Discover proven methods to remove dark spots on your face. Learn about causes, treatments, and prevention from medical experts.
April 23, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.
April 20, 2026

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026