Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Learn about MRSA, how it spreads, its symptoms, and crucial precautions to prevent these antibiotic-resistant staph infections in community and healthcare settings.

Methicillin-resistant Staphylococcus aureus (MRSA) is a type of bacteria that can cause infections that are difficult to treat because they are resistant to many common antibiotics. While MRSA infections can occur anywhere, they are most frequently found in healthcare settings like hospitals and nursing homes. However, they can also spread in the community, particularly among people who have close skin-to-skin contact. Understanding how MRSA spreads and taking the right precautions is crucial for preventing infections in yourself and others. What is MRSA? MRSA stands for Methicillin-resistant Staphylococcus aureus. It is a specific type of bacteria, commonly known as 'staph,' that has developed resistance to certain antibiotics, including methicillin and other common antibiotics like oxacillin, penicillin, and amoxicillin. Staph bacteria are very common and can live on the skin or in the nose of many healthy people without causing any problems. However, when these bacteria enter the body through a cut or wound, they can cause infections. How Does MRSA Spread? MRSA spreads through direct contact with an infected person or by touching contaminated objects and surfaces. The mode of transmission can differ slightly between community settings and healthcare facilities. Community Spread: Contact with personal items: Sharing items like towels, razors, clothing, or athletic equipment that have come into contact with MRSA bacteria can lead to spread. Contact with wounds: Touching an open wound or sore that is infected with MRSA can transmit the bacteria. Close physical contact: Activities involving frequent skin-to-skin contact, such as in sports, can increase the risk of transmission. Healthcare Setting Spread: Contaminated surfaces and equipment: MRSA can survive on surfaces and medical equipment that have not been properly cleaned and disinfected. Healthcare professionals: Transmission can occur from healthcare workers to patients if proper hygiene protocols, like handwashing and glove use, are not followed. Invasive devices: Patients who have invasive medical devices such as urinary catheters or intravenous (IV) lines are at higher risk, as these can serve as entry points for MRSA into the body. Who is at Risk for MRSA? While anyone can develop an MRSA infection, certain groups are at higher risk: Hospital patients: Individuals in hospitals, especially those with weakened immune systems or who have undergone surgery or have invasive devices. Residents of long-term care facilities: Similar to hospitals, these settings can facilitate the spread of MRSA. People with weakened immune systems: Conditions like HIV/AIDS, cancer, or those undergoing chemotherapy can make individuals more susceptible. Individuals with chronic illnesses: Such as diabetes or kidney disease. Intravenous (IV) drug users: Sharing needles and having direct contact with bacteria can significantly increase the risk. Athletes and those in close contact: People involved in contact sports or living in close quarters (like dormitories) are at increased risk due to frequent skin-to-skin contact. People with skin injuries: Cuts, scrapes, or surgical wounds provide an entry point for bacteria. Symptoms of MRSA Infection MRSA infections often start as small, red bumps that resemble pimples or boils. These bumps can quickly develop into painful, deep abscesses. Other symptoms may include: Redness and swelling around the affected area. Warmth to the touch. Pus or drainage from the wound. Fever. Pain at the site of infection. In more severe cases, MRSA can spread deeper into the body, causing serious infections like pneumonia, bloodstream infections (sepsis), or infections of the heart valves (endocarditis). These severe infections can be life-threatening. Diagnosis of MRSA If a doctor suspects a MRSA infection, they will typically take a sample of the infected material (such as pus from a wound or a swab from the nose) and send it to a laboratory for testing. This test will identify the specific type of bacteria and determine which antibiotics are effective against it. Treatment for MRSA Treating MRSA infections can be challenging due to their antibiotic resistance. The treatment approach depends on the severity and location of the infection: Drainage of abscesses: For skin infections, the first step is often to drain the pus from the abscess. Antibiotics: If antibiotics are needed, doctors will prescribe specific ones that are known to be effective against MRSA. These may include vancomycin, clindamycin, doxycycline, or trimethoprim-sulfamethoxazole. It is crucial to complete the entire course of antibiotics as prescribed, even if symptoms improve. Hospitalization: Severe or invasive MRSA infections often require hospitalization for intravenous antibiotic treatment and close monitoring. Precautions to Prevent MRSA Spread Preventing the spread of MRSA relies on good hygiene practices and specific precautions, especially in healthcare settings. The Centers for Disease Control and Prevention (CDC) recommends standard contact precautions. In the Community: Practice good hand hygiene: Wash your hands frequently with soap and water for at least 20 seconds, or use an alcohol-based hand sanitizer if soap and water are not available. Keep wounds clean and covered: Clean any cuts or scrapes thoroughly and cover them with a clean bandage. Change bandages regularly. Avoid sharing personal items: Do not share towels, razors, clothing, or athletic equipment. Disinfect surfaces: Regularly clean and disinfect frequently touched surfaces, especially if someone in the household has an infection. Shower after sports: If you participate in contact sports, shower immediately after practice or games and wash your athletic gear. In Healthcare Settings: Handwashing: Healthcare professionals must wash their hands thoroughly before and after patient contact, and after touching the patient's surroundings. Use of gloves and gowns: Healthcare workers should wear gloves and gowns when entering the room of a patient with MRSA to prevent
In summary, timely diagnosis, evidence-based treatment, and prevention-focused care improve long-term health outcomes.
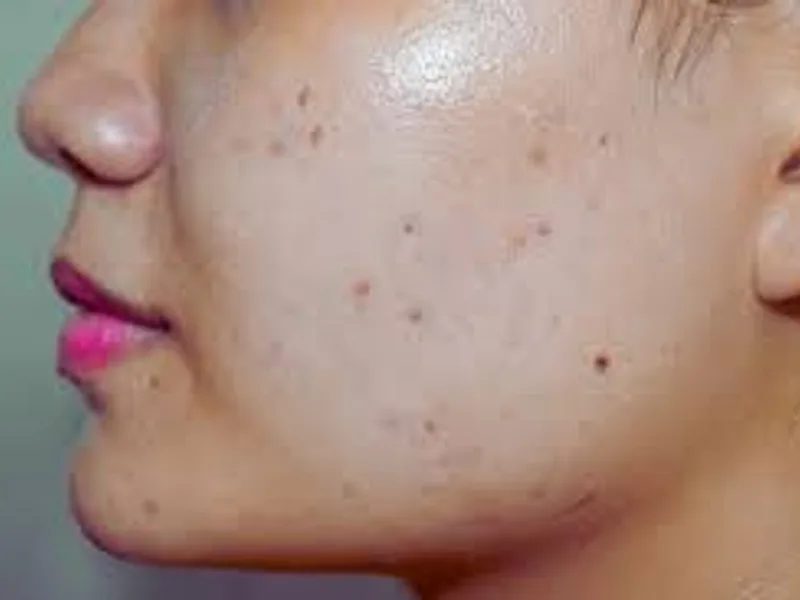
Discover proven methods to remove dark spots on your face. Learn about causes, treatments, and prevention from medical experts.
April 23, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.
April 20, 2026

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026