Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Learn about Middle East Respiratory Syndrome (MERS), a viral respiratory illness caused by MERS-CoV. Understand its symptoms, causes, diagnosis, treatment, and crucial prevention strategies. Find out when to consult a doctor and get answers to common questions.

Middle East Respiratory Syndrome (MERS) is a viral respiratory illness caused by a coronavirus known as MERS-CoV. It is a zoonotic virus, meaning it can be transmitted between animals and humans. While it was first identified in Saudi Arabia in 2012, it has since been diagnosed in numerous countries, primarily in the Middle East, Africa, and South Asia. Most confirmed cases have been linked to individuals who have traveled to or had contact with someone from the Arabian Peninsula. MERS is a serious illness that primarily affects the lungs and airways, and in severe cases, can lead to organ damage and has a significant mortality rate, with approximately 35% of diagnosed individuals succumbing to the illness, often due to underlying health conditions.
It's important to understand that MERS is caused by a different coronavirus than the one that causes COVID-19 (SARS-CoV-2). However, the research conducted on MERS and SARS (Severe Acute Respiratory Syndrome) has been instrumental in the rapid development of diagnostics, treatments, and vaccines for COVID-19. While MERS is not as widespread as COVID-19, knowing about its symptoms, transmission, and prevention is crucial, especially for those planning to travel to regions where MERS has been identified.
Symptoms of MERS typically appear within 5 to 6 days after exposure to the virus, but the incubation period can range from 2 to 14 days. While some individuals may experience no symptoms, most people infected with MERS will exhibit a range of flu-like symptoms. These can include:
In addition to respiratory symptoms, some individuals may also experience gastrointestinal issues such as:
In severe cases, MERS can lead to serious complications, including pneumonia and kidney failure. The severity of symptoms can vary greatly from person to person, influenced by factors such as age and underlying health conditions.
The primary cause of MERS is the MERS coronavirus (MERS-CoV). This virus is believed to have originated in bats and then transmitted to dromedary camels, which serve as an intermediate host. The most common route of human infection is through direct or indirect contact with infected dromedary camels. This can occur through:
Human-to-human transmission of MERS is also possible, though less common than animal-to-human transmission. This typically occurs in healthcare settings among close contacts of infected individuals or within households where someone has MERS. The risk of transmission is higher in situations with prolonged close contact and inadequate infection control measures.
Diagnosing MERS involves a combination of clinical evaluation, travel history, and laboratory testing. If a doctor suspects MERS, they will typically:
Early and accurate diagnosis is vital for initiating appropriate treatment and preventing further spread of the virus.
Currently, there is no specific antiviral treatment approved for MERS. Treatment is primarily supportive, focusing on managing symptoms and complications. This may include:
In some cases, experimental treatments or medications used for other viral infections may be considered under strict medical supervision. It is essential to seek medical attention promptly if you suspect you have MERS.
Preventing MERS involves taking precautions to avoid exposure to the virus, particularly if you are in or traveling to regions where MERS is prevalent. Key preventive measures include:
Adhering to these preventive measures can significantly reduce the risk of contracting and spreading MERS.
You should consult a doctor immediately if you develop symptoms suggestive of MERS, especially if you have recently traveled to the Middle East or had close contact with someone diagnosed with MERS or a sick camel. Prompt medical attention is crucial for accurate diagnosis, appropriate treatment, and to prevent the spread of the virus. If you experience severe respiratory distress, high fever, or other concerning symptoms, do not delay in seeking professional medical help.
Yes, both MERS and COVID-19 are caused by coronaviruses. However, they are caused by different specific viruses: MERS by MERS-CoV and COVID-19 by SARS-CoV-2. While they share similarities as respiratory illnesses, they have different origins, transmission patterns, and severity.
Yes, MERS can be transmitted from person to person, primarily through close contact with an infected individual, especially in healthcare settings or households. However, human-to-human transmission is less common than transmission from camels to humans.
The World Health Organization (WHO) reports that approximately 35% of people diagnosed with MERS have died. However, many of these individuals had underlying health conditions that weakened their immune systems.
While possible, the risk of contracting MERS from consuming camel meat is significantly reduced if the meat is thoroughly cooked. It is advisable to avoid raw or undercooked camel meat.
As of now, there are no approved vaccines for MERS. Research and development for vaccines are ongoing, but none are currently available for public use.
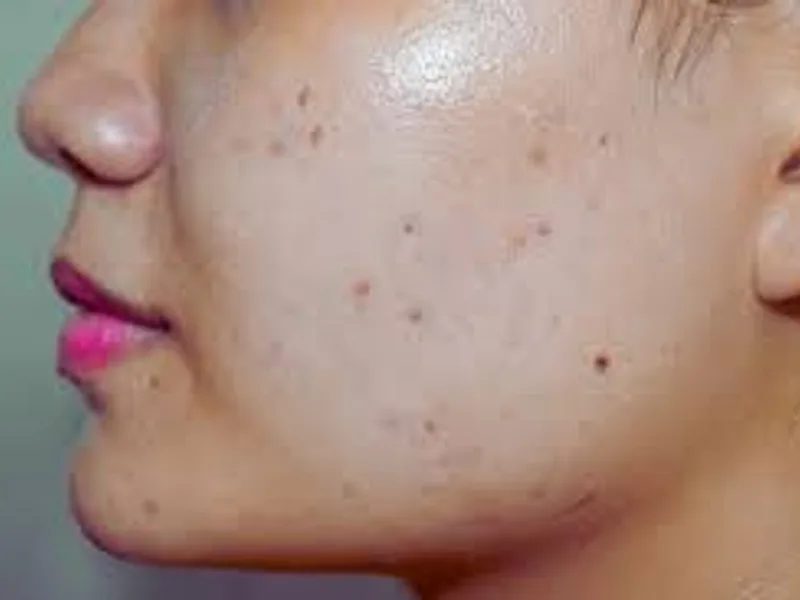
Discover proven methods to remove dark spots on your face. Learn about causes, treatments, and prevention from medical experts.
April 23, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.
April 20, 2026

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026