Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Explore the connection between the common herpes simplex virus (HSV) and ulcerative colitis (UC). Understand how immunosuppressive treatments for UC can increase the risk of HSV complications like herpes simplex virus colitis, its symptoms, diagnosis, and treatment.

Inflammatory Bowel Disease (IBD), which includes conditions like ulcerative colitis (UC) and Crohn's disease, affects millions worldwide. While managing these chronic conditions, patients often undergo treatments that can suppress their immune system. This suppression, while beneficial for controlling IBD symptoms, can inadvertently increase the risk of opportunistic infections. One such concern is the potential link between the herpes simplex virus (HSV) and a severe complication known as herpes simplex virus colitis, particularly in individuals with ulcerative colitis.
Herpes simplex virus is a common viral infection that affects a significant portion of the global population. There are two primary types:
It's important to note that HSV is widespread. Globally, an estimated 67% of people have contracted HSV-1, and around 13% have contracted HSV-2. Once contracted, the virus often remains dormant in the body, with the potential to reactivate under certain conditions.
Herpes simplex virus colitis is a rare but serious condition where the herpes simplex virus causes inflammation in the colon (large intestine). This condition is particularly concerning for individuals with IBD, such as ulcerative colitis. The virus can exacerbate existing inflammation in the bowel, leading to severe symptoms and complications.
The connection between HSV and ulcerative colitis primarily stems from the treatments used for IBD. Many IBD treatments involve immunosuppressant medications. These drugs work by dampening the immune system's response to reduce inflammation in the gut. However, a suppressed immune system is less effective at fighting off infections, making individuals more vulnerable to opportunistic pathogens like HSV.
When an individual with IBD, especially one on immunosuppressants, contracts HSV or has a dormant HSV infection reactivate, it can lead to herpes simplex virus colitis. The virus can directly infect the cells of the colon, triggering an inflammatory response that worsens the underlying colitis. This can lead to a more severe and difficult-to-manage disease flare-up.
Herpes simplex virus colitis does not develop spontaneously. It requires two main factors:
The risk is significantly heightened in individuals with IBD who are on immunosuppressive therapy. Medications such as corticosteroids, thiopurines, and biologic agents, while crucial for managing IBD, can compromise the immune system's ability to control viral activity. This can lead to either a new HSV infection or the reactivation of a previously dormant virus, potentially resulting in herpes simplex virus colitis.
While HSV is common, herpes simplex virus colitis is a rare complication. The primary risk factor is having IBD, particularly when combined with:
Many individuals infected with HSV show no symptoms. When symptoms do appear, they can range from mild to severe. For those with a compromised immune system, symptoms can be more pronounced.
General HSV Symptoms:
Symptoms Specific to Herpes Simplex Virus Colitis:
These symptoms often overlap with general ulcerative colitis flare-ups but can be more severe:
It is crucial to recognize that these symptoms can indicate a worsening of IBD or a new complication, necessitating prompt medical evaluation.
Diagnosing herpes simplex virus colitis involves a combination of clinical evaluation and laboratory tests. While antibody tests can confirm past exposure to HSV, they are not reliable for diagnosing an active infection causing colitis.
The diagnostic process typically includes:
Early and accurate diagnosis is vital for effective treatment.
The primary treatment for herpes simplex virus colitis involves antiviral medications. These drugs help to suppress the virus and reduce its replication, thereby alleviating inflammation and symptoms.
It is essential to follow the prescribed treatment plan diligently and communicate any concerns or side effects to your healthcare provider.
Preventing herpes simplex virus colitis primarily focuses on minimizing the risk of HSV infection and managing IBD effectively:
If you have ulcerative colitis or another form of IBD and experience a sudden worsening of your symptoms, especially if they include:
It is crucial to seek immediate medical attention. These symptoms could indicate a serious complication like herpes simplex virus colitis, and prompt diagnosis and treatment are essential to prevent severe outcomes.
Q1: Can everyone with ulcerative colitis get herpes simplex virus colitis?
No, it is a rare complication. It primarily affects individuals with IBD who are on immunosuppressive therapy and contract or reactivate the herpes simplex virus.
Q2: Is herpes simplex virus colitis contagious?
The herpes simplex virus itself is contagious through direct contact with sores or infected bodily fluids. However, herpes simplex virus colitis is a complication within the colon and is not directly transmitted from person to person in that form.
Q3: Can IBD treatment be stopped if I get herpes simplex virus colitis?
Treatment decisions are complex and made on a case-by-case basis by your doctor. Sometimes, IBD medications might be adjusted or temporarily paused, but this is carefully weighed against the risks of uncontrolled IBD.
Q4: How long does treatment for herpes simplex virus colitis last?
The duration of antiviral treatment varies but typically lasts for a specific course prescribed by your doctor, often ranging from a few weeks to a couple of months, depending on the severity and response.
Q5: Can herpes simplex virus colitis lead to long-term damage?
If left untreated or if it is very severe, herpes simplex virus colitis can lead to complications such as bowel strictures, fistulas, or toxic megacolon. Prompt treatment significantly reduces the risk of long-term damage.
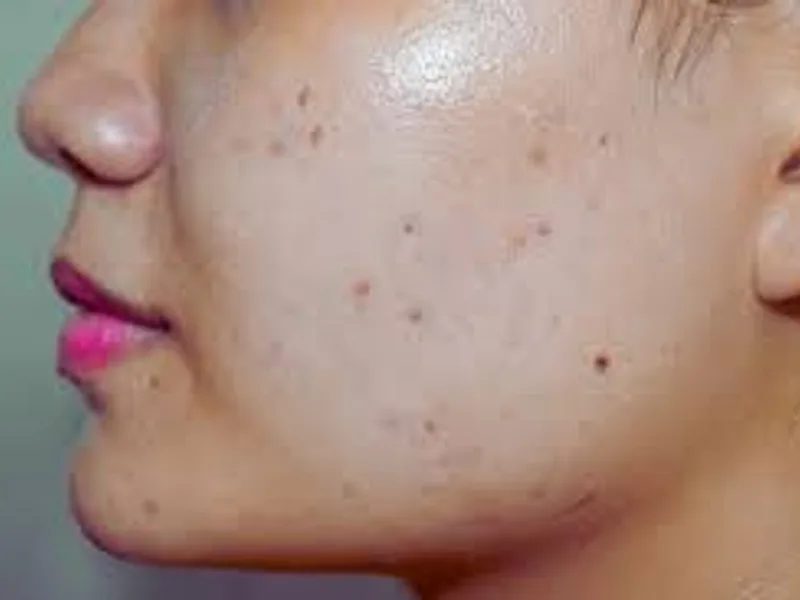
Discover proven methods to remove dark spots on your face. Learn about causes, treatments, and prevention from medical experts.
April 23, 2026

Understand the peripheral blood smear test for malaria diagnosis, its procedure, and what results mean for patients.
April 20, 2026

Discover how specialized staining techniques, like Giemsa, are crucial for accurately diagnosing Leishmaniasis, identifying the parasite, and guiding timely treatment. Understand this key diagnostic approach.
April 20, 2026