Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand your fundamental right to decline medical treatment. Learn how to communicate your decisions effectively, the role of informed consent, legal implications, and how to ensure your healthcare choices align with your personal values and beliefs.
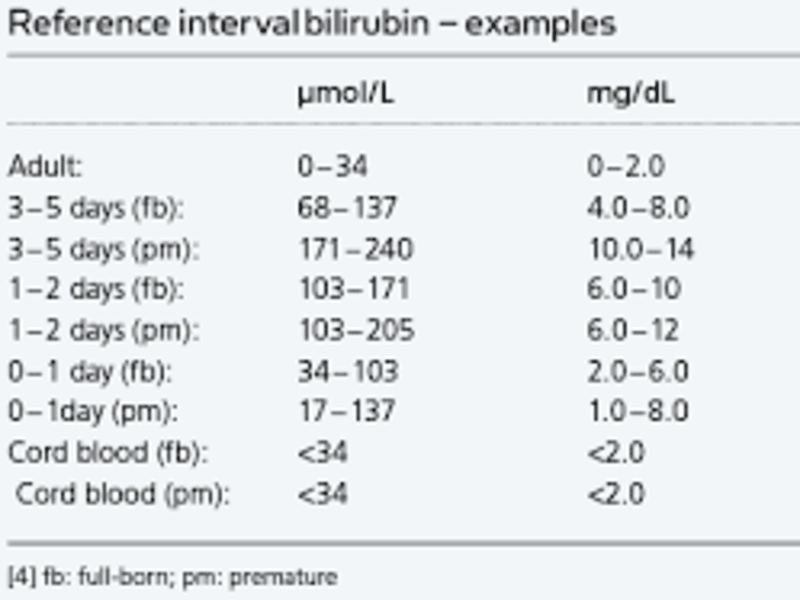
Bilirubin levels help assess liver health. This guide explains normal bilirubin values, types, causes of abnormal levels, symptoms, and when to seek medical advice.
April 11, 2026

Learn how to properly clean and care for your new ear piercing to ensure it heals beautifully and avoid infection. Follow our step-by-step guide for optimal results.
April 1, 2026


Navigating the complex world of healthcare often involves making crucial decisions about your well-being. While doctors are highly trained professionals dedicated to providing the best care, you, as the patient, hold the ultimate authority over your body and your health choices. This fundamental principle, known as patient autonomy, grants you the right to accept or decline any proposed medical treatment, even if it goes against your doctor's recommendation. Understanding this right and knowing how to communicate your decisions effectively is vital for an empowered healthcare journey.
This comprehensive guide will delve into the intricacies of declining medical treatment, exploring your rights, the ethical considerations involved, and practical steps for communicating your choices clearly and respectfully with your healthcare providers. We aim to equip you with the knowledge to make informed decisions that align with your values, beliefs, and personal health goals.
Before discussing the right to decline treatment, it's essential to understand its counterpart: informed consent. Informed consent is a cornerstone of medical ethics and law, ensuring that patients have all the necessary information to make voluntary decisions about their medical care. It's not just a signature on a form; it's a dynamic process of communication between you and your healthcare provider.
Your healthcare provider's role is to act as an expert guide, offering their professional opinion and recommendations based on their knowledge and experience. They are ethically bound to present all relevant information fairly and objectively. When you express a desire to decline treatment, their responsibility shifts from advocating for a specific treatment to ensuring you fully understand the implications of your decision.
The right to self-determination in healthcare is enshrined in legal and ethical codes globally. It affirms that competent adults have the moral and legal right to refuse medical treatment, even if that refusal could lead to serious harm or death. This right is a direct extension of patient autonomy.
Patient autonomy means that you have the right to make decisions about your own body and health, free from external control. It recognizes your unique values, beliefs, and life goals, which may not always align with purely medical objectives. For example, a patient might prioritize quality of life over extending life at all costs, or their religious beliefs might prohibit certain medical interventions.
You can decline any medical treatment at any stage, provided you are a competent adult. This includes:
It's important to note that declining one treatment does not mean declining all care. You can still seek other forms of care, palliative care, or choose different treatment options.
Patients decline medical treatment for a multitude of personal and complex reasons. Understanding these motivations can foster empathy and facilitate better communication between patients and providers.
Many treatments, especially for serious illnesses, come with significant side effects that can severely impact a patient's daily life, comfort, and independence. Fear of pain, nausea, fatigue, hair loss, cognitive impairment, or long-term disability can be powerful motivators for declining treatment.
Some patients may choose to pursue alternative or complementary therapies instead of, or in conjunction with, conventional medical treatments. This decision often stems from a belief in the efficacy of these methods, a desire for a more natural approach, or dissatisfaction with conventional options.
Healthcare costs can be exorbitant, even with insurance. Patients may decline treatments due to concerns about their ability to afford co-pays, deductibles, or treatments not covered by their plan. Beyond direct costs, practical challenges such as transportation to appointments, childcare, time off work, or lack of local support systems can also influence decisions.
A breakdown in the doctor-patient relationship, previous negative experiences with the healthcare system, or a lack of trust in the physician's recommendations can lead a patient to decline treatment. Furthermore, if the patient doesn't fully understand their condition, the proposed treatment, or the alternatives, they may feel unable to give truly informed consent and opt to refuse.
Communicating your decision to decline treatment can be challenging, especially when your doctor strongly believes in a particular course of action. Clear, respectful, and assertive communication is key to ensuring your wishes are understood and respected.
Before your appointment, take time to reflect on your reasons for declining treatment. Write down your concerns, questions, and what you hope to achieve (or avoid). This will help you articulate your position clearly.
State your decision directly and politely. For example, you might say, "Doctor, I appreciate your recommendation, but after careful consideration, I've decided not to proceed with [specific treatment] at this time." Avoid vague language or apologies that might suggest you're unsure.
Even if you're declining a specific treatment, engage in dialogue. Ask your doctor to explain the potential consequences of your refusal, any alternative options that might be available, or what signs you should look for that might indicate a need for different intervention. Understanding the risks associated with declining treatment is part of making an informed decision.
If you're unsure or want to confirm your decision, don't hesitate to request a second opinion. A fresh perspective from another qualified physician can provide additional information, validate your concerns, or offer alternative approaches you hadn't considered.
Having a trusted family member or friend with you can be incredibly helpful. They can offer emotional support, help you remember what was discussed, and advocate on your behalf if you feel overwhelmed.
When you decline medical treatment, there are certain implications and procedures that your healthcare team will follow.
Your doctor will document your decision to decline treatment in your medical record. This documentation typically includes: the recommended treatment, the risks and benefits of the recommended treatment, the risks and benefits of declining treatment (including doing nothing), and your expressed reasons for refusal. This is crucial for legal and ethical reasons, demonstrating that informed consent was sought and refusal was made voluntarily.
In some situations, particularly in a hospital setting, if you choose to leave or refuse a critical treatment that your healthcare team believes is essential for your immediate safety or recovery, you may be asked to sign an 'Against Medical Advice' (AMA) form. This form acknowledges that you understand the potential risks of your decision and are releasing the hospital and medical staff from liability for any adverse outcomes resulting from your refusal. Signing an AMA form does not mean you are giving up your right to future care.
It is paramount that you understand the potential health consequences of declining treatment. Your doctor is obligated to explain these risks clearly, which could range from worsening of your condition, irreversible damage, increased pain, or even death. While you have the right to refuse, you also have the right to be fully informed about the potential impact of that refusal.
Even if you decline treatment, your doctor still has ethical obligations to you. These include: respecting your autonomous decision, providing information about alternative options (even if they don't personally endorse them), continuing to offer palliative or supportive care, and ensuring a smooth transition of care if you choose to seek treatment elsewhere.
The right to decline treatment is deeply rooted in broader legal and ethical principles.
The right to refuse treatment hinges on the patient's capacity or competency to make decisions. A competent adult is presumed to have the ability to understand information, appreciate the consequences of their choices, and communicate their decision. If a patient is deemed incompetent (e.g., due to severe dementia, unconsciousness, or acute mental health crisis), decisions may fall to a legally appointed surrogate (like a durable power of attorney for healthcare) or be made in the patient's best interest by the medical team, often with legal oversight.
Advance directives are legal documents that allow you to express your healthcare wishes in advance, in case you become unable to make decisions for yourself. They are powerful tools for ensuring your autonomy is respected even when you cannot speak for yourself.
Discussing and documenting your wishes through advance directives is a proactive step in exercising your right to decline treatment.
While adults generally have an unfettered right to refuse treatment, there are exceptions:
Declining treatment is a significant decision, and it's always wise to remain open to further discussion or even reconsideration if circumstances change.
If you find yourself second-guessing your decision, feeling pressured, or experiencing significant anxiety, it's a sign to revisit the conversation with your doctor or seek additional perspectives. It's okay to change your mind.
Medical science evolves, and new treatment options may emerge. Your condition might also change, making previously unsuitable treatments more viable, or vice versa. Stay informed and discuss any new developments with your healthcare team.
If your health significantly deteriorates or improves in an unexpected way, the balance of risks and benefits for treatments you previously declined might shift. Be proactive in discussing these changes and their implications for your treatment choices.
A doctor cannot refuse to care for you simply because you declined a specific treatment, especially if you still require medical attention. However, if your refusal makes it impossible for the doctor to provide appropriate care according to their professional standards, they may ethically and legally withdraw from your care, provided they give you reasonable notice and help you find another provider. They cannot abandon you.
Often, yes. While not always legally required, healthcare providers typically ask you to sign a form acknowledging your decision to decline treatment. This form documents that you were informed of the risks and benefits and made your decision voluntarily. It protects both you (by documenting your wishes) and the provider (by demonstrating informed refusal).
You have the right to change your mind at any time, as long as you are competent. Inform your healthcare provider immediately of your decision to accept treatment, and they will proceed accordingly, provided the treatment is still medically appropriate and available.
No, if you are a competent adult, your family or next of kin cannot override your decision to decline treatment, even if they disagree with it. Your autonomy takes precedence. However, if you are deemed incompetent, a legally appointed healthcare proxy (chosen by you in an advance directive) or a court-appointed guardian would make decisions on your behalf.
Yes, there are limited exceptions. These typically involve situations where your decision poses a significant threat to public health (e.g., highly contagious diseases) or when a minor's life is at stake and parental refusal is deemed neglectful. These situations are rare and often involve legal intervention.
The right to decline medical treatment is a powerful expression of your autonomy and self-determination. It underscores the essential truth that healthcare is a collaborative process, not a directive. By understanding your rights, communicating openly and assertively with your healthcare team, and planning for future eventualities through advance directives, you can navigate your medical journey with confidence and ensure that your healthcare decisions truly reflect your values and wishes. Remember, your voice matters, and your choices are paramount in your personal health narrative.
This article is based on general principles of medical ethics, patient rights, and informed consent widely recognized in healthcare law and practice. For specific legal advice or detailed information on your local healthcare regulations, please consult with a legal professional or your healthcare provider.
Discover practical, science-backed tips to sharpen your reaction time for gaming, sports, and everyday life. Learn how to improve your brain's speed and accuracy.
April 1, 2026