Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand misdiagnosis, its prevalence, and impact. Learn about the causes of diagnostic errors, from cognitive biases to systemic issues, and discover actionable strategies to advocate for your health, recognize red flags, and prevent misdiagnosis for accurate care.

In the intricate world of healthcare, receiving an accurate diagnosis is the cornerstone of effective treatment and recovery. However, the path to a correct diagnosis is not always straightforward. Misdiagnosis, a critical issue within modern medicine, occurs when a patient receives an incorrect diagnosis, a delayed diagnosis, or no diagnosis at all for a condition they have. This can lead to significant health consequences, emotional distress, and financial burdens. Understanding misdiagnosis – its causes, its impact, and how to prevent it – is crucial for every patient navigating the healthcare system.
This comprehensive guide from Doctar aims to shed light on the multifaceted problem of misdiagnosis. We will explore what constitutes a misdiagnosis, its prevalence, the various factors that contribute to diagnostic errors, and most importantly, equip you with actionable strategies to advocate for yourself and ensure you receive the accurate care you deserve.
Misdiagnosis is an umbrella term encompassing several types of diagnostic errors:
Diagnostic errors are not always due to negligence; they can arise from complex interactions between physician cognition, systemic factors, and the inherent challenges of medical science.
Misdiagnosis is a more pervasive problem than many realize. Studies have consistently highlighted its significant incidence:
These statistics underscore the urgent need for greater awareness and proactive strategies to improve diagnostic accuracy across the healthcare landscape.
While you might not be able to diagnose yourself, you can learn to recognize signs that your current diagnosis might be flawed or incomplete. Trust your instincts and pay attention to these red flags:
If you've been following your doctor's treatment plan diligently, but your symptoms are not improving, are getting worse, or new symptoms are appearing, it's a significant indicator that the initial diagnosis might be incorrect or incomplete. Effective treatment should yield some positive change.
The emergence of new, unexplained symptoms or a significant worsening of your existing symptoms, especially if they don't align with the expected progression of your diagnosed condition, should prompt further investigation. Your body might be trying to tell you something different.
If you've consulted multiple doctors and received differing opinions or diagnoses without a clear explanation for the discrepancies, it's a strong signal to dig deeper. Different specialties may view symptoms through different lenses, but a stark contradiction warrants further clarity.
Sometimes, a diagnosis just doesn't resonate with your experience. If you feel that your symptoms are being shoehorned into a particular condition, or if the explanation for your illness feels incomplete or unconvincing, don't dismiss that feeling. Your lived experience of your symptoms is invaluable.
If your doctor is unable to clearly explain your diagnosis, the reasoning behind it, or the proposed treatment plan in a way you can understand, it can be a sign of diagnostic uncertainty or a communication breakdown. You have a right to comprehensible information about your health.
If you feel that your concerns are being minimized, your symptoms are not being taken seriously, or your doctor is not listening attentively to your full story, it can lead to crucial information being missed. A good doctor-patient relationship is built on mutual respect and open communication.
Diagnostic errors are rarely due to a single factor. They typically arise from a complex interplay of human cognitive processes, systemic healthcare challenges, and unique patient presentations.
Doctors, like all humans, are susceptible to cognitive biases, which are systematic errors in thinking that can influence judgment and decision-making. Some common biases contributing to misdiagnosis include:
The healthcare system itself can create environments conducive to diagnostic errors:
Sometimes, aspects related to the patient can also complicate the diagnostic process:
Diagnosing rare diseases poses a particular challenge. Physicians may have limited experience with these conditions, and their symptoms often mimic more common illnesses, leading to prolonged diagnostic odysseys for patients.
No diagnostic test is 100% accurate. False positives and false negatives can occur, and the interpretation of test results can be subjective. Over-reliance on technology without clinical correlation can also lead to errors.
The consequences of misdiagnosis can be far-reaching and devastating, affecting patients physically, emotionally, and financially.
When diagnostic errors occur, it not only impacts the individual patient but can also contribute to a broader erosion of public trust in the healthcare system, hindering effective health-seeking behaviors.
While healthcare professionals bear the primary responsibility for accurate diagnosis, patients can play a vital role in advocating for their own health and minimizing the risk of misdiagnosis. Becoming an informed and proactive participant in your care is one of your most powerful tools.
Preparation is key to effective communication and ensuring all relevant information is shared:
Clear and honest communication is paramount:
Seeking a second opinion is a common and often recommended practice, not a sign of distrust. It can provide fresh perspectives and confirm or challenge an initial diagnosis. When to seek one:
Ask your current doctor for a referral or seek out a specialist independently. Ensure all relevant medical records are transferred to the new physician.
Take an active role in understanding your condition:
Keep a personal file of all your medical information, including test results, doctor's notes, medication lists, and summaries of appointments. This can be invaluable if you need to consult new doctors or seek a second opinion.
For complex cases or if you feel overwhelmed, consider hiring a professional patient advocate. These individuals can help you navigate the healthcare system, understand your options, and communicate with providers on your behalf.
Knowing when to act is crucial. Consider consulting your doctor or seeking a second opinion if:
Q: Can misdiagnosis be considered medical malpractice?
A: Not all misdiagnoses constitute medical malpractice. Malpractice typically involves negligence, meaning a healthcare professional failed to meet the accepted standard of care, and this failure directly resulted in harm to the patient. A misdiagnosis becomes malpractice if a reasonably competent doctor in the same field would not have made the same error under similar circumstances, and that error caused injury or damage. It's a complex legal area, and consulting with a legal professional specializing in medical malpractice is recommended if you suspect this is the case.
Q: How do I get a second opinion?
A: You can ask your current doctor for a referral to another specialist. Most doctors understand and support patients seeking second opinions, especially for serious conditions. Alternatively, you can research specialists independently through hospital websites, professional organizations, or online directories. When seeking a second opinion, ensure you have all your relevant medical records (test results, imaging scans, doctor's notes) to provide to the new physician.
Q: What should I do if I suspect I've been misdiagnosed?
A: First, gather all your medical records. Review your symptoms, their timeline, and any treatments you've received. Prepare a clear list of your concerns and questions. Schedule an appointment with your current doctor to express your concerns and ask for further investigation or a referral. If you're still not satisfied, seek a second opinion from another specialist. Document every interaction and decision.
Q: Are certain conditions more prone to misdiagnosis?
A: Yes. Conditions with vague, non-specific, or overlapping symptoms are often misdiagnosed. Examples include fibromyalgia, chronic fatigue syndrome, Lyme disease, autoimmune disorders, and certain mental health conditions. Additionally, conditions that are rare or present atypically can be challenging to diagnose correctly. The "big three" serious conditions most often involved in misdiagnosis are cancer, vascular events (like heart attack or stroke), and infections.
Q: What role does technology play in preventing misdiagnosis?
A: Technology plays an increasingly vital role. Advanced imaging (MRI, CT scans), sophisticated lab tests, and genetic sequencing can provide more precise diagnostic information. Artificial intelligence (AI) and machine learning are being developed to assist clinicians by analyzing vast amounts of data, identifying patterns, and flagging potential diagnostic errors. Telemedicine can also improve access to specialists, particularly in rural areas, potentially reducing diagnostic delays. However, technology is a tool and requires skilled human interpretation.
Misdiagnosis is a serious challenge in healthcare, but it is not an insurmountable one. By understanding its potential causes and impacts, and by actively engaging in your own healthcare journey, you can significantly reduce your risk. Remember that you are your own best advocate. Don't be afraid to ask questions, seek clarification, and pursue second opinions when necessary. Your proactive involvement in your diagnosis and treatment is not just your right, but a powerful step towards ensuring accurate care and safeguarding your health. Doctar is committed to empowering you with the knowledge and tools to navigate your health journey with confidence.
This article's content is based on information from reputable medical institutions, peer-reviewed studies, and expert consensus in the field of diagnostic medicine and patient safety. Key references include reports from the National Academies of Sciences, Engineering, and Medicine (NASEM), the Agency for Healthcare Research and Quality (AHRQ), and leading medical journals focusing on diagnostic error research.
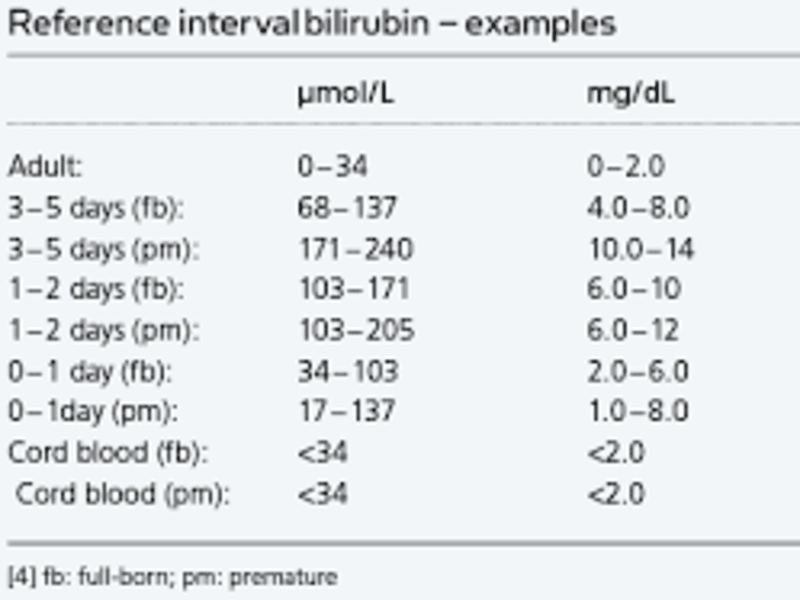
Bilirubin levels help assess liver health. This guide explains normal bilirubin values, types, causes of abnormal levels, symptoms, and when to seek medical advice.
April 11, 2026

Learn how to properly clean and care for your new ear piercing to ensure it heals beautifully and avoid infection. Follow our step-by-step guide for optimal results.
April 1, 2026

Discover practical, science-backed tips to sharpen your reaction time for gaming, sports, and everyday life. Learn how to improve your brain's speed and accuracy.
April 1, 2026