Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Discover comprehensive strategies to reduce your risk of age-related macular degeneration (AMD). Learn about symptoms, causes, diagnosis, treatment, and crucial prevention tips through diet, lifestyle, and regular eye care. Safeguard your vision for the future with this expert guide.
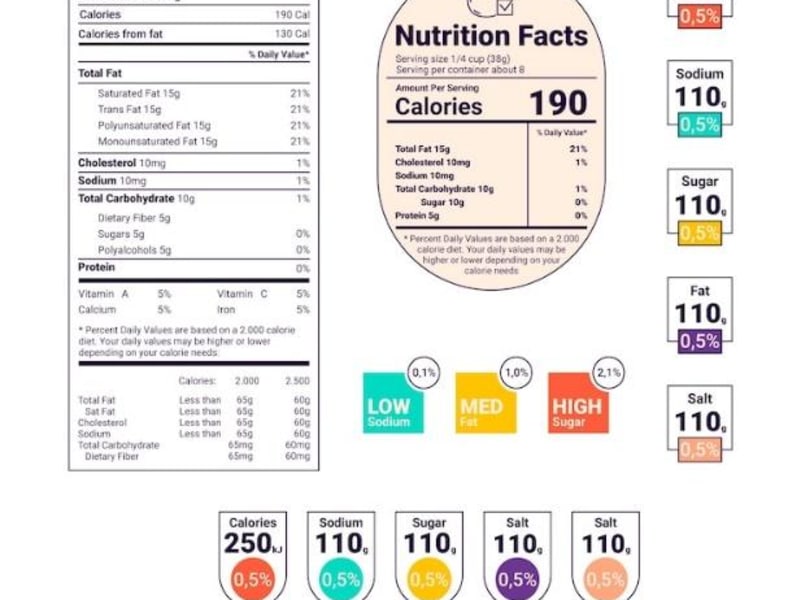
Nutrition labels are designed to inform — but food manufacturers often make them difficult to interpret. This expert guide walks through every section of a nutrition label, exposing the common tricks used to mislead consumers and showing you what to actually look for.
April 14, 2026
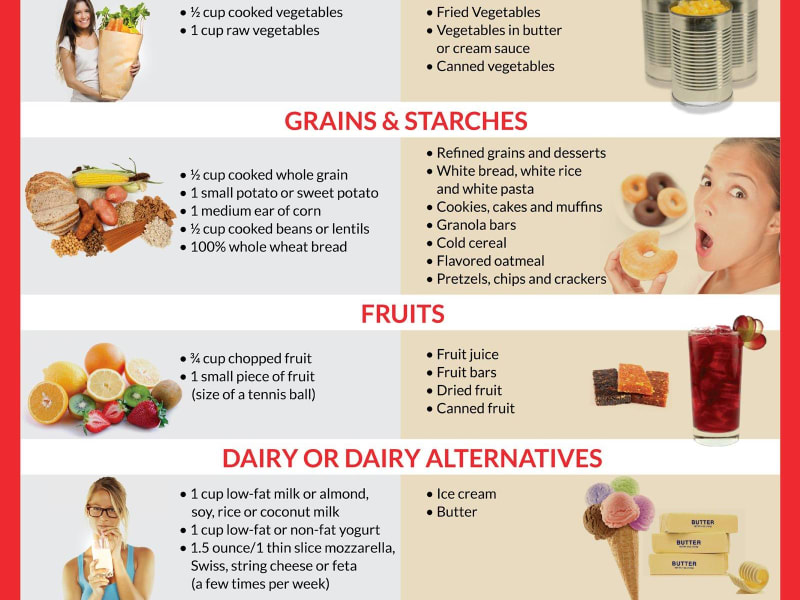
The carbohydrate debate is more nuanced than "eat less carbs." The quality of carbohydrates — their fibre content, processing level, and glycaemic impact — matters far more than their mere presence in your diet. Here's the science behind the distinction.
April 14, 2026


Age-related Macular Degeneration (AMD) is a progressive eye condition that stands as a leading cause of severe, irreversible vision loss among individuals aged 50 and older. It specifically targets the macula, a small but critical part of the retina responsible for sharp, central vision, which is essential for tasks like reading, driving, and recognizing faces. While AMD can significantly impair quality of life, the good news is that numerous proactive steps can be taken to reduce your risk of developing this condition or slow its progression. This comprehensive guide from Doctar aims to empower you with the knowledge and actionable strategies needed to protect your precious eyesight. We will delve into understanding AMD, its symptoms, causes, diagnosis, and available treatments, but our primary focus will be on the powerful role of prevention through diet, lifestyle, and consistent eye care.
To truly grasp AMD, it's vital to understand the macula. Located in the center of the retina at the back of the eye, the macula is a highly sensitive area densely packed with photoreceptor cells (cones) that are responsible for perceiving fine details and color vision. It allows us to see objects directly in front of us with clarity. When AMD develops, this crucial area begins to deteriorate. The condition is broadly categorized into two main types:
AMD affects millions worldwide, and its prevalence is expected to rise as the global population ages. It is the leading cause of irreversible blindness and severe vision impairment in developed countries. The impact extends beyond just vision loss; individuals with AMD often experience difficulties with daily activities, leading to reduced independence, increased risk of falls, and even symptoms of depression and anxiety due to the profound lifestyle changes necessitated by the condition. Early detection and proactive prevention are therefore paramount to mitigating its devastating effects.
Recognizing the early signs of AMD is crucial for timely intervention. While early-stage dry AMD might not present noticeable symptoms, regular eye exams can detect drusen before vision is affected. As the condition progresses, symptoms become more apparent:
It's important to note that AMD typically affects central vision, while peripheral (side) vision usually remains intact. This is why individuals with advanced AMD may still be able to navigate their surroundings but struggle with tasks requiring fine detail.
While the exact cause of AMD is complex and not fully understood, a combination of genetic, environmental, and lifestyle factors is believed to contribute to its development and progression. Some key risk factors include:
This is the most significant risk factor. AMD is, by definition, age-related. The risk dramatically increases after the age of 50, and it becomes more common with each decade of life.
If you have a close relative (parent, sibling) with AMD, your risk is significantly higher. Researchers have identified several genes linked to AMD, particularly those involved in the immune system (e.g., Complement Factor H – CFH) and lipid metabolism (e.g., ARMS2). Genetic predisposition doesn't guarantee AMD but increases susceptibility.
Smoking is unequivocally the strongest modifiable risk factor for AMD. Smokers are at a two to four times higher risk of developing AMD compared to non-smokers. It also accelerates the progression of the disease. Toxins in cigarette smoke damage retinal cells, impair blood flow to the eyes, and increase oxidative stress.
A diet lacking in essential vitamins, minerals, and antioxidants can increase AMD risk. Conversely, a diet rich in fruits, vegetables, and omega-3 fatty acids has been shown to be protective.
Studies suggest that obesity increases the risk of developing advanced AMD and can accelerate its progression. This is likely due to the systemic inflammation and oxidative stress associated with excess body fat.
Conditions like high blood pressure (hypertension), high cholesterol, and atherosclerosis (hardening of the arteries) can impair blood flow to the eyes, potentially contributing to AMD development or worsening.
Prolonged exposure to ultraviolet (UV) light and certain wavelengths of blue light from the sun may contribute to retinal damage and increase AMD risk over a lifetime. While the evidence is not as strong as for smoking, protection is generally recommended.
Caucasians appear to be at a higher risk of developing AMD compared to individuals of African or Hispanic descent. However, AMD can affect people of all racial and ethnic backgrounds.
Some studies suggest that women may have a slightly higher risk of developing AMD, possibly due to longer life expectancy.
Early diagnosis of AMD, especially before significant vision loss occurs, is critical for effective management and slowing progression. Regular, comprehensive eye exams are the cornerstone of detection, particularly for individuals over 50 or those with risk factors.
An ophthalmologist or optometrist will perform a thorough eye examination. This typically includes:
This simple, square grid with a dot in the center is a vital tool for self-monitoring at home and for initial clinical assessment. If you have AMD, straight lines on the grid may appear wavy, broken, or distorted, or you might notice a dark spot. Regular use of the Amsler grid can help detect subtle changes in central vision, prompting an earlier visit to the eye care specialist.
OCT is a non-invasive imaging test that uses light waves to create high-resolution cross-sectional images of your retina. It's like an ultrasound for the eye, providing detailed views of the retinal layers, detecting fluid accumulation, drusen, and abnormal blood vessels. OCT is invaluable for diagnosing and monitoring both dry and wet AMD and assessing treatment efficacy.
If wet AMD is suspected, FA may be performed. A dye (fluorescein) is injected into a vein in your arm, which travels to the blood vessels in your eye. A special camera then takes rapid photographs as the dye passes through the retina. This reveals any abnormal blood vessels, leakage, or blockages, precisely pinpointing the source of the problem in wet AMD.
Digital photographs of the retina can be taken to document the current state of the macula. These images serve as a baseline for comparison in future visits, helping to track the progression of drusen or other changes over time.
While there is currently no cure for AMD, especially dry AMD, various treatments and management strategies can help preserve vision, slow progression, or even improve vision, particularly for wet AMD.
Currently, there is no medical treatment to reverse or cure dry AMD. However, its progression can often be slowed, especially in intermediate to advanced stages, with specific nutritional supplements.
These supplements are generally recommended for individuals with intermediate AMD in one or both eyes, or advanced AMD in one eye. It's crucial to consult with your eye care professional before starting any new supplement regimen, as high doses of certain vitamins can have side effects or interact with other medications.
Wet AMD requires prompt and ongoing medical intervention to prevent severe and rapid vision loss.
Regular follow-up appointments and ongoing treatment are vital for managing wet AMD, as the abnormal blood vessels can recur.
While some risk factors like age and genetics are beyond our control, a significant portion of AMD risk is modifiable through conscious lifestyle choices. Embracing these preventative strategies can empower you to protect your vision for years to come.
What you eat plays a profound role in eye health. A diet rich in specific nutrients can help protect the macula from oxidative damage and inflammation.
Beyond diet, several lifestyle choices significantly impact your AMD risk.
Protecting your eyes from environmental damage is a simple yet effective preventative step.
Even if you have no symptoms, regular comprehensive dilated eye exams are crucial for early detection and prevention.
If AMD runs in your family, inform your eye care professional. This awareness allows for earlier and more frequent screenings, potentially catching the disease at its earliest, most manageable stages.
Prompt medical attention is vital if you experience any changes in your vision that could indicate AMD or its progression. Do not delay seeking professional help. You should see an ophthalmologist immediately if you notice:
Even without symptoms, if you are over 50 or have risk factors for AMD, schedule regular comprehensive dilated eye exams as recommended by your eye care professional.
A: Unfortunately, there is currently no cure for AMD. However, treatments for wet AMD can often stabilize vision, prevent further loss, and sometimes even improve vision. For dry AMD, specific nutritional supplements (AREDS2 formula) can slow its progression in intermediate stages.
A: Yes, there are two main types: dry (atrophic) AMD, which is more common and progresses slowly, and wet (neovascular) AMD, which is less common but can cause rapid and severe vision loss due to abnormal blood vessel growth and leakage.
A: The Amsler grid is a simple tool used for self-monitoring central vision. It's a square grid with a dot in the center. To use it, cover one eye, look directly at the center dot, and note if any lines appear wavy, broken, or if there are any dark spots. Repeat with the other eye. If you notice any changes, contact your eye doctor immediately.
A: While eye exercises can help with eye strain or improve eye muscle coordination in some cases, there is no scientific evidence to suggest that they prevent or treat macular degeneration.
A: No, it's never too late. If you have early or intermediate dry AMD, adopting a healthy lifestyle, including a nutrient-rich diet and considering AREDS2 supplements (under medical guidance), can significantly reduce your risk of progression to advanced AMD.
A: The role of blue light from digital screens in causing AMD is still a subject of ongoing research. However, prolonged exposure to high-energy blue light, particularly from the sun, is believed to contribute to retinal damage over a lifetime. Protecting your eyes with UV-blocking sunglasses and considering blue light filters for screens is a prudent preventative measure.
A: Genetics play a significant role. If you have a close family member with AMD, your risk is increased. Several genes have been identified that are associated with a higher risk of developing the condition. If you have a strong family history, it's even more important to be proactive with prevention and regular eye exams.
A: Both cataracts and AMD can cause blurred vision, but they affect different parts of the eye and present with distinct symptoms. Cataracts cause clouding of the eye's lens, leading to generally hazy or cloudy vision and glare sensitivity. AMD affects the macula, causing central vision distortion or a blind spot. It's possible to have both conditions simultaneously, and an eye doctor can accurately diagnose each.
Age-related Macular Degeneration is a formidable challenge to vision health, but it is not an insurmountable one. By understanding its nature, recognizing its early signs, and, most importantly, embracing a proactive approach to prevention, you hold significant power in safeguarding your central vision. The journey to reducing your AMD risk begins with informed choices: nourishing your body with an eye-healthy diet rich in antioxidants and omega-3s, adopting a smoke-free and active lifestyle, protecting your eyes from harmful UV and blue light, and committing to regular comprehensive eye examinations. These simple yet profound steps can make a monumental difference in preserving the clarity and vibrancy of your world. Remember, your vision is a precious gift – invest in its protection today for a clearer tomorrow. Consult with your eye care professional to tailor a personalized prevention and monitoring plan that best suits your individual needs and risk profile.
Most official protein recommendations were set to prevent deficiency — not to optimise health, muscle mass, or longevity. New research suggests the real requirements are significantly higher than the standard RDA, particularly for active adults and older populations.
April 13, 2026