Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Explore the gluten-free diet's pros and cons for those without celiac disease or intolerance. Learn about medical necessities, trendy motivations, potential benefits, and risks like nutritional deficiencies. Get expert advice on when to consider a gluten-free trial and how to approach it safely, focusing on whole foods and professional guidance.
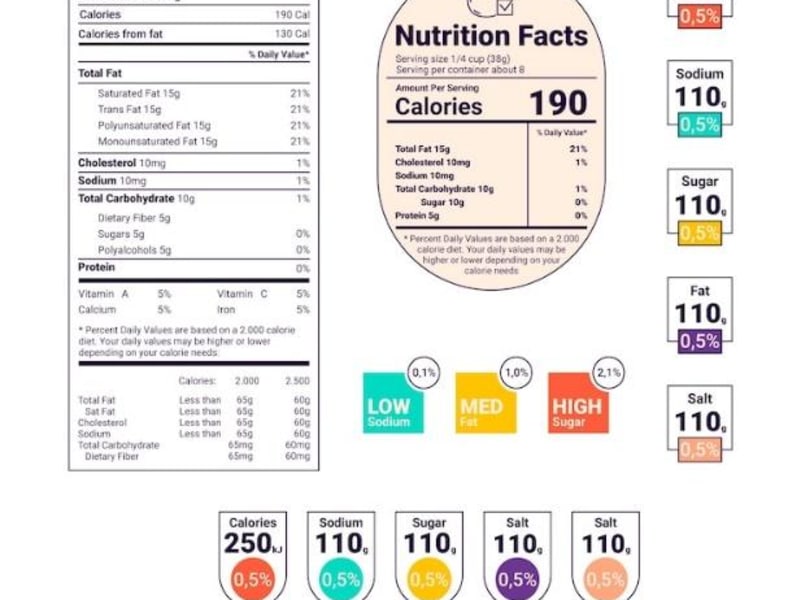
Nutrition labels are designed to inform — but food manufacturers often make them difficult to interpret. This expert guide walks through every section of a nutrition label, exposing the common tricks used to mislead consumers and showing you what to actually look for.
April 14, 2026
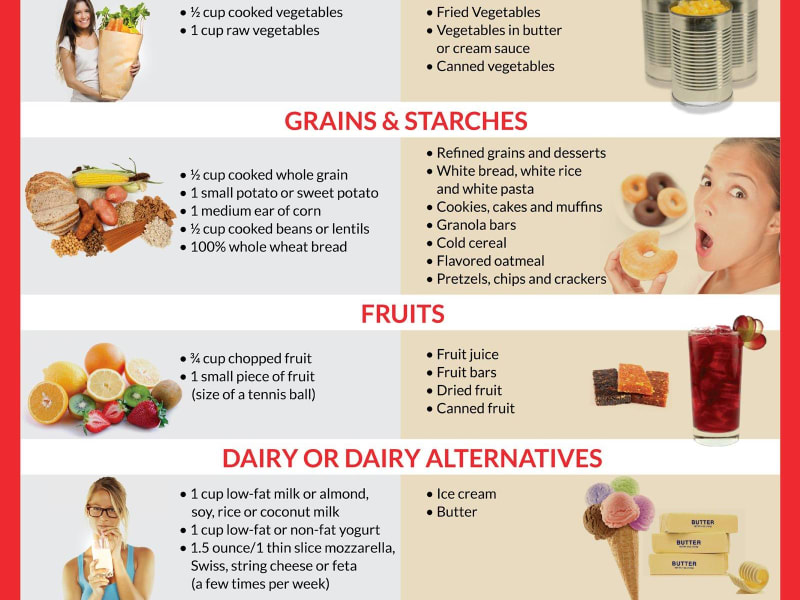
The carbohydrate debate is more nuanced than "eat less carbs." The quality of carbohydrates — their fibre content, processing level, and glycaemic impact — matters far more than their mere presence in your diet. Here's the science behind the distinction.
April 14, 2026


The term "gluten-free" has become a ubiquitous buzzword in health and wellness circles, adorning food labels, restaurant menus, and social media feeds. What started as a necessary medical intervention for a specific group of individuals has evolved into a widespread dietary trend, embraced by many who do not have a diagnosed gluten intolerance. This article aims to demystify the gluten-free diet, exploring who truly needs it, why others choose to adopt it, and the potential benefits and risks associated with going gluten-free without a medical necessity. We will delve into the science, symptoms, diagnosis, and practical implications to help you make an informed decision about your dietary choices.
For individuals with celiac disease, a gluten-free diet is not a choice but a lifelong medical requirement. However, for the vast majority of the population, gluten consumption poses no health threat. The growing popularity of gluten-free eating among those without a medical diagnosis raises important questions about its actual health benefits, potential downsides, and whether it's truly a path to better health for everyone.
Before diving into the diet itself, it's crucial to understand what gluten is. Gluten is not a single compound but a general name for the proteins found in wheat (including spelt, farro, durum, semolina, and triticale), barley, and rye. The two main proteins in gluten are gliadin and glutenin.
Gluten plays a vital role in food production, particularly in baking. It acts as a binder, providing elasticity to dough and giving bread its chewy texture and ability to rise. Without gluten, baked goods tend to be crumbly and less pliable, which is why gluten-free baking often requires a combination of different flours and starches to mimic these properties.
Understanding gluten's role and sources is the first step in navigating a gluten-free diet, whether by necessity or choice. It's important to remember that gluten is naturally present in many staple foods worldwide, and its historical consumption is deeply ingrained in human diets.
For certain individuals, avoiding gluten is not a dietary preference but a critical medical treatment to prevent severe health complications. The primary conditions necessitating a strict gluten-free diet are celiac disease, non-celiac gluten sensitivity, and wheat allergy. Each of these conditions has distinct mechanisms, symptoms, and diagnostic approaches.
What it is: Celiac disease is a serious autoimmune disorder where the ingestion of gluten leads to damage in the small intestine. When someone with celiac disease consumes gluten, their immune system mistakenly attacks the villi—tiny, finger-like projections lining the small intestine responsible for nutrient absorption. This damage, known as villous atrophy, impairs the body's ability to absorb nutrients, leading to a wide range of health problems. Celiac disease has a genetic component, meaning individuals are predisposed to it, and it can be triggered at any age.
Symptoms: Celiac disease is often called a "great imitator" because its symptoms can be highly varied and affect almost every organ system. While some individuals experience classic digestive symptoms, many have non-digestive or "silent" symptoms. The severity and type of symptoms can also vary greatly among individuals.
Diagnosis: Accurate diagnosis of celiac disease is crucial and involves a multi-step process. It is absolutely vital that individuals continue to eat gluten throughout the diagnostic process; stopping gluten prematurely can lead to false-negative results, making diagnosis impossible without reintroducing gluten (a "gluten challenge").
Treatment: The only effective treatment for celiac disease is a strict, lifelong gluten-free diet. Even small amounts of gluten can cause intestinal damage and symptoms. Adherence to the diet allows the small intestine to heal, symptoms to resolve, and nutrient absorption to improve, significantly reducing the risk of long-term complications.
What it is: NCGS, sometimes referred to as gluten sensitivity or non-celiac wheat sensitivity, describes a condition where individuals experience symptoms similar to celiac disease after consuming gluten, but without the autoimmune response, intestinal damage, or allergic reaction characteristic of celiac disease or wheat allergy. The exact mechanisms behind NCGS are not fully understood, and research is ongoing. It is believed that components other than gluten in wheat, such as FODMAPs (fermentable oligosaccharides, disaccharides, monosaccharides, and polyols), might play a role in some cases.
Symptoms: NCGS symptoms often overlap significantly with those of celiac disease and irritable bowel syndrome (IBS). They typically appear hours or days after gluten ingestion and resolve when gluten is removed from the diet, reappearing upon reintroduction.
Diagnosis: There is currently no specific biomarker or diagnostic test for NCGS. It is a diagnosis of exclusion. This means that celiac disease and wheat allergy must first be definitively ruled out by appropriate medical testing. Once these conditions are excluded, a healthcare professional may recommend an elimination diet followed by a controlled gluten challenge:
Treatment: A gluten-free diet is the recommended treatment for NCGS. However, unlike celiac disease, individuals with NCGS may not need to be as strictly gluten-free and might be able to tolerate small amounts of gluten or gluten from specific sources. The level of restriction is often tailored to the individual's symptom threshold.
What it is: A wheat allergy is an immune system reaction to one or more of the many proteins found in wheat, not just gluten. It is a classic food allergy, meaning the body's immune system mistakenly identifies wheat proteins as a threat and mounts an allergic response, typically involving IgE antibodies. This is distinct from celiac disease (an autoimmune response) and NCGS (which doesn't involve an allergic or autoimmune response).
Symptoms: Symptoms of a wheat allergy typically appear rapidly, within minutes to a few hours after consuming wheat. They can range from mild to severe and, in some cases, can be life-threatening.
Diagnosis: Diagnosis of a wheat allergy typically involves:
Treatment: The primary treatment for wheat allergy is strict avoidance of wheat and wheat-containing products. Individuals with a history of severe reactions are prescribed an epinephrine auto-injector and educated on its use. It's important to note that avoiding wheat does not necessarily mean avoiding all gluten-containing grains (like barley or rye), although many individuals find it easier to avoid all sources of gluten to ensure no wheat contamination.
Beyond medical necessity, a significant portion of the population has adopted a gluten-free diet as a lifestyle choice. This trend has been fueled by a combination of factors, including pervasive marketing, celebrity endorsements, anecdotal success stories, and a general perception that gluten-free equals healthier. Let's explore the common reasons people choose this diet without a formal diagnosis.
Many individuals embark on a gluten-free journey believing it will unlock a host of health improvements, even if they don't have celiac disease or NCGS.
The gluten-free trend has been amplified by powerful external forces:
It's crucial to approach these perceived benefits with a critical eye and understand that correlation does not equal causation. While people may feel better on a gluten-free diet, it doesn't automatically mean gluten was the culprit for their previous symptoms. Often, the improvements are a side effect of a broader shift towards healthier eating habits.
While a gluten-free diet is essential for those with celiac disease or severe gluten sensitivity, adopting it without a medical reason can carry significant risks and drawbacks. It's not a universally healthier diet and can lead to various nutritional, financial, and social challenges.
Gluten-containing whole grains are vital sources of numerous essential nutrients. Eliminating them without careful planning can lead to deficiencies:
The rise of the gluten-free trend has led to an explosion of processed gluten-free products. While these offer convenience, they are often not healthier than their gluten-containing counterparts:
Gluten-free specialty products are typically significantly more expensive than their gluten-containing equivalents. Maintaining a strictly gluten-free diet can place a considerable financial burden on individuals and families, especially if they rely heavily on packaged GF alternatives rather than naturally gluten-free whole foods.
Adopting a restrictive diet can have social and emotional repercussions:
Self-diagnosing gluten intolerance and adopting a gluten-free diet without medical consultation can be dangerous:
These risks highlight the importance of medical consultation before making significant and potentially unnecessary dietary changes.
Given the potential downsides, a gluten-free diet should not be undertaken lightly or without careful consideration. However, for individuals who experience persistent digestive or systemic symptoms and have ruled out celiac disease and wheat allergy, a carefully managed trial of a gluten-free diet under professional guidance might be considered. This approach helps in identifying potential sensitivities without risking nutritional deficiencies or delayed diagnosis of other conditions.
The absolute first step is to consult your doctor and, ideally, a registered dietitian (RD) or a nutritionist specializing in digestive health. They can help:
If you decide to try a gluten-free diet, prioritize naturally gluten-free whole foods over processed gluten-free alternatives. This strategy maximizes nutrient intake and avoids the pitfalls of unhealthy processed GF products.
Gluten can hide in unexpected places. If you're going strictly gluten-free, you'll need to become an expert label reader. Look for
Most official protein recommendations were set to prevent deficiency — not to optimise health, muscle mass, or longevity. New research suggests the real requirements are significantly higher than the standard RDA, particularly for active adults and older populations.
April 13, 2026