In the bustling world of health and wellness, trends come and go, often promising quick fixes for complex problems. One such trend that frequently surfaces is the idea of a "3-day gut reset" or "gut cleanse." The allure of rapidly improving digestive health and overall well-being in just a few days is undeniably strong. But is it truly possible to fundamentally reset your gut microbiome in such a short timeframe? And what does a doctor actually recommend for sustainable gut health?
At Doctar, we believe in providing evidence-based information to empower you to make informed decisions about your health. In this comprehensive guide, we'll delve into the science behind gut health, dissect the concept of a rapid gut reset, and, most importantly, share what actually works, according to medical experts, to cultivate a thriving gut microbiome for long-term health. Forget the fleeting fads; let's explore practical, sustainable strategies endorsed by doctors.
Understanding Your Gut Microbiome: The Foundation of Health
Before we can discuss resetting or improving gut health, it's crucial to understand what the gut microbiome is and why it plays such a pivotal role in our overall well-being.
What is the Gut Microbiome?
Your gut microbiome is a complex ecosystem of trillions of microorganisms, including bacteria, viruses, fungi, and other microbes, primarily residing in your large intestine. Far from being mere passengers, these microbes are active participants in numerous bodily functions. Each person's microbiome is unique, influenced by genetics, diet, lifestyle, environment, and early life exposures.
Why is a Healthy Gut Important?
A balanced and diverse gut microbiome is fundamental to health. Its functions extend far beyond digestion:
- Digestion and Nutrient Absorption: Gut microbes help break down food components that your body can't digest on its own, such as certain fibers. They also produce essential vitamins, including vitamin K and several B vitamins, and influence the absorption of minerals.
- Immune System Regulation: A significant portion of your immune system (around 70-80%) resides in your gut. A healthy microbiome helps train and regulate immune responses, protecting against pathogens and preventing autoimmune reactions.
- Metabolism and Weight Management: The gut microbiome influences how your body stores fat, balances blood sugar levels, and responds to hormones that regulate appetite. Imbalances have been linked to obesity and metabolic syndrome.
- Brain Health and Mood: The "gut-brain axis" is a bidirectional communication system between the gut and the brain. Gut microbes produce neurotransmitters like serotonin (a mood regulator) and influence brain function, impacting mood, cognition, and even susceptibility to conditions like anxiety and depression.
- Inflammation Control: A healthy gut barrier and a balanced microbiome prevent harmful substances from entering the bloodstream, thus reducing systemic inflammation, which is a root cause of many chronic diseases.
- Protection Against Pathogens: A diverse community of beneficial bacteria occupies ecological niches, making it harder for harmful bacteria to establish themselves and cause infection.
The "3-Day Gut Reset" Trend: Fact vs. Fiction
The concept of a rapid gut reset often involves restrictive diets, juice cleanses, specific supplements, or fasting protocols, all promising to "detox" or "reboot" the digestive system quickly. While the intention behind these trends is often good, the scientific reality is more nuanced.
What Does a "Gut Reset" Typically Involve?
Common elements of a trendy 3-day gut reset might include:
- Elimination Diets: Temporarily cutting out common allergens or inflammatory foods like gluten, dairy, sugar, and processed foods.
- Juice Cleanses: Consuming only juices (often raw, cold-pressed) for a few days, purportedly to give the digestive system a rest.
- Specific Supplements: Taking high doses of probiotics, prebiotics, digestive enzymes, or herbal detox blends.
- Fasting Protocols: Short-term intermittent fasting or prolonged fasting.
- High-Fiber Intake: Emphasizing fruits, vegetables, and whole grains, sometimes in liquid form.
Can You Truly "Reset" Your Gut in 3 Days?
From a scientific standpoint, the idea of a complete "reset" of the gut microbiome in just three days is largely a misconception. While short-term dietary changes can certainly induce shifts in the microbial population, these changes are often temporary and superficial, particularly if followed by a return to previous unhealthy habits.
Dr. Emily Johnson, a gastroenterologist at Doctar-affiliated hospital, explains, "Your gut microbiome is a complex, resilient ecosystem that has developed over years. While you can certainly influence its composition with dietary changes, a fundamental 'reset' that brings about lasting improvements in just 72 hours is highly unlikely. Think of it more like fine-tuning rather than a complete overhaul. Sustainable change requires consistent, long-term effort."
Studies have shown that diet can rapidly alter the gut microbiome composition within days. However, these changes are often transient. For example, a shift to an animal-based diet or a plant-based diet can quickly change which bacteria are abundant, but these changes tend to revert once the original diet is resumed. True, beneficial, and lasting changes to the diversity and function of the gut microbiome typically require weeks to months of consistent effort.
Moreover, aggressive "cleanses" can sometimes do more harm than good, potentially stripping away beneficial bacteria along with harmful ones, or leading to nutrient deficiencies and electrolyte imbalances, especially if not supervised by a healthcare professional.
Common Symptoms of an Unhealthy Gut
An imbalanced gut microbiome, or dysbiosis, can manifest in a variety of ways, affecting not just your digestive system but also other parts of your body. Recognizing these symptoms is the first step toward addressing gut health.
Digestive Symptoms
- Bloating and Gas: Excessive gas production and abdominal bloating are common signs, often due to certain bacteria fermenting undigested food.
- Diarrhea or Constipation: Irregular bowel movements, ranging from persistent loose stools to chronic constipation, can indicate an imbalance in gut motility and microbial activity.
- Abdominal Pain and Cramping: Discomfort, pain, or cramping in the abdomen without an obvious cause.
- Heartburn or Acid Reflux: While often associated with diet, gut dysbiosis can contribute to issues with stomach acid regulation.
- Nausea: Persistent feelings of sickness or an upset stomach.
- Food Intolerances: Developing sensitivities to foods you previously tolerated well.
Non-Digestive Symptoms
The gut-brain axis and the gut-immune axis mean that gut health can impact nearly every system in the body.
- Fatigue and Low Energy: Poor nutrient absorption and chronic inflammation from an unhealthy gut can lead to persistent tiredness.
- Skin Issues: Conditions like acne, eczema, and psoriasis have been linked to gut dysbiosis and increased gut permeability ("leaky gut").
- Mood Changes: Anxiety, depression, irritability, and brain fog can be influenced by the gut microbiome's production of neurotransmitters and its impact on inflammation.
- Unexplained Weight Changes: Difficulty losing weight or unexplained weight gain can sometimes be tied to gut microbial imbalances affecting metabolism.
- Autoimmune Conditions: Emerging research suggests a strong link between gut health and the development or exacerbation of autoimmune diseases.
- Frequent Infections: A compromised gut microbiome can weaken the immune system, leading to more frequent colds, flu, or other infections.
- Poor Sleep Quality: The gut microbiome influences the production of melatonin, a hormone crucial for sleep.
Causes of Gut Imbalance (Dysbiosis)
Many factors contribute to an unhealthy gut microbiome. Understanding these causes is essential for effective prevention and treatment.
Diet and Lifestyle Factors
- Poor Diet: A diet high in processed foods, sugar, unhealthy fats, and low in fiber and diverse plant foods is a primary driver of dysbiosis. These foods often feed harmful bacteria while starving beneficial ones.
- Lack of Dietary Diversity: A limited range of plant-based foods means a limited range of fibers and prebiotics, which are essential for supporting a diverse microbiome.
- Excessive Alcohol Consumption: Alcohol can irritate the gut lining and negatively alter microbial composition.
- Lack of Physical Activity: Regular exercise has been shown to positively impact gut microbial diversity.
- Chronic Stress: Stress directly affects the gut-brain axis, altering gut motility, permeability, and microbial composition.
- Insufficient Sleep: Sleep deprivation can disrupt circadian rhythms, which in turn can affect gut health.
Medications and Medical Conditions
- Antibiotics: While essential for bacterial infections, antibiotics indiscriminately kill both harmful and beneficial bacteria, leading to significant, though often temporary, disruptions in the microbiome.
- Proton Pump Inhibitors (PPIs): These medications, used to reduce stomach acid, can alter the gut environment, potentially leading to bacterial overgrowth in the small intestine and dysbiosis.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Prolonged use of NSAIDs can damage the gut lining, increasing permeability.
- Chronic Diseases: Conditions like inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), diabetes, and autoimmune disorders are often associated with gut dysbiosis, though the exact cause-and-effect relationship can be complex.
Stress and Environment
- Environmental Toxins: Exposure to pesticides, pollutants, and other environmental toxins can negatively impact gut health.
- Infections: Past gastrointestinal infections can sometimes leave lasting changes in the gut microbiome.
- Aging: The diversity of the gut microbiome tends to decrease with age, which can contribute to various age-related health issues.
Diagnosing Gut Issues
If you suspect you have gut health issues, it's important to consult with a healthcare professional. Self-diagnosis and self-treatment, especially with aggressive "cleanses," can be ineffective or even harmful.
What Your Doctor Might Do
Your doctor will typically start with a thorough medical history and physical examination. They will ask about your symptoms, diet, lifestyle, medications, and any family history of digestive disorders. They may also ask about stool consistency and frequency.
Diagnostic Tests
Depending on your symptoms and medical history, your doctor might recommend one or more of the following tests:
- Stool Tests: These can identify infections, inflammation markers, malabsorption, and sometimes provide insights into microbial balance, though direct microbiome analysis is still largely a research tool.
- Blood Tests: To check for inflammation markers (e.g., C-reactive protein), nutrient deficiencies (e.g., iron, vitamin B12), or antibodies related to celiac disease or other autoimmune conditions.
- Breath Tests: Used to diagnose conditions like small intestinal bacterial overgrowth (SIBO) or lactose intolerance.
- Endoscopy or Colonoscopy: In cases of persistent or severe symptoms, these procedures allow direct visualization of the digestive tract and tissue biopsies to check for inflammation, ulcers, or other abnormalities.
- Imaging Studies: X-rays, CT scans, or MRI may be used to rule out structural issues.
It's important to remember that while some direct-to-consumer gut microbiome tests are available, their clinical utility and actionable insights are still debated within the medical community. Always discuss these with your doctor.
Evidence-Based Strategies for Long-Term Gut Health (Beyond 3 Days)
While a quick "reset" might not be realistic, adopting sustainable, evidence-based strategies can significantly improve your gut health over time. These approaches focus on nurturing a diverse and balanced microbiome.
Dietary Interventions
Diet is the single most powerful lever you have for shaping your gut microbiome.
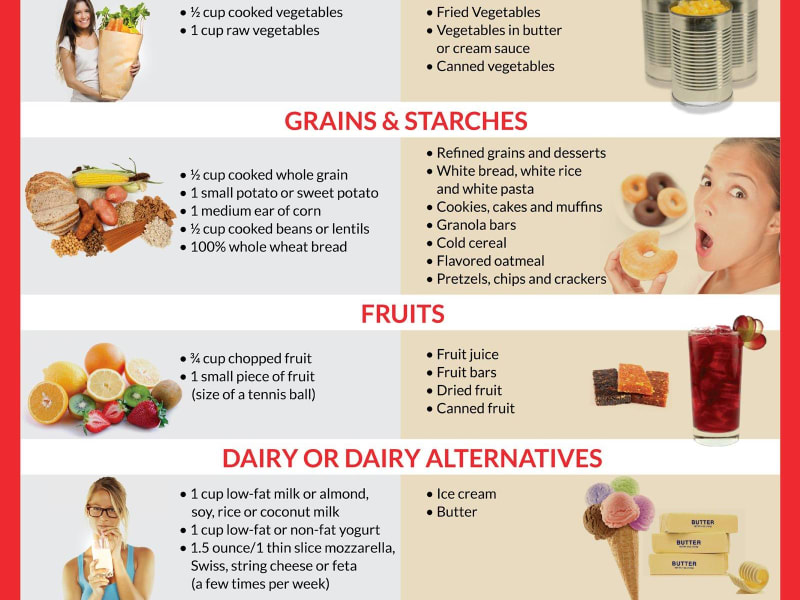
- Fiber-Rich Foods: Fiber is the primary food source for beneficial gut bacteria. Aim for a wide variety of plant-based foods.
- Fruits: Berries, apples, pears, bananas.
- Vegetables: Broccoli, spinach, kale, carrots, artichokes, asparagus, onions, garlic.
- Legumes: Lentils, beans, chickpeas.
- Whole Grains: Oats, barley, quinoa, brown rice.
- Nuts and Seeds: Almonds, walnuts, flaxseeds, chia seeds.
These foods provide diverse types of fiber (soluble, insoluble, resistant starch) that feed different strains of bacteria, promoting diversity.
- Fermented Foods: These foods naturally contain live beneficial bacteria (probiotics) and their metabolic byproducts. Incorporate them regularly.
- Yogurt and Kefir: Choose plain, unsweetened varieties with live and active cultures.
- Sauerkraut and Kimchi: Fermented cabbage products.
- Kombucha: A fermented tea.
- Tempeh and Miso: Fermented soybean products.
Start with small amounts and gradually increase to avoid digestive discomfort.
- Limiting Processed Foods, Sugar, and Artificial Sweeteners: These ingredients can negatively impact gut diversity and promote the growth of less beneficial bacteria.
- Processed Foods: Often low in fiber and high in unhealthy fats and additives.
- Added Sugars: Can feed harmful bacteria and contribute to inflammation.
- Artificial Sweeteners: Some studies suggest they can negatively alter the microbiome.
Focus on whole, unprocessed foods as much as possible.
- Include Healthy Fats: Omega-3 fatty acids found in fatty fish (salmon, mackerel), flaxseeds, and walnuts have anti-inflammatory properties that can benefit gut health.
- Stay Hydrated: Water is essential for maintaining gut motility and softening stool, aiding in regular bowel movements.
Lifestyle Adjustments
Beyond diet, lifestyle factors play a crucial role in gut health.
- Stress Management: Chronic stress can wreak havoc on your gut. Incorporate stress-reducing practices into your daily routine.
- Mindfulness and Meditation: Even 10-15 minutes a day can make a difference.
- Yoga or Tai Chi: Gentle physical activity combined with breathing techniques.
- Spending Time in Nature: "Forest bathing" has been shown to reduce stress hormones.
- Deep Breathing Exercises: Simple techniques to calm the nervous system.
- Regular Exercise: Moderate physical activity can increase gut microbial diversity and improve gut motility. Aim for at least 150 minutes of moderate-intensity exercise per week.
- Adequate Sleep: Poor sleep can disrupt the gut microbiome and increase inflammation. Prioritize 7-9 hours of quality sleep per night. Establish a consistent sleep schedule and create a relaxing bedtime routine.
- Avoid Unnecessary Antibiotics: Only take antibiotics when medically necessary, and always complete the full course as prescribed. Discuss with your doctor about ways to support your gut during and after antibiotic treatment, such as taking probiotics.
Targeted Supplements (When Appropriate)
While a food-first approach is ideal, certain supplements can be beneficial under the guidance of a healthcare professional.
- Probiotics: Live microorganisms that, when administered in adequate amounts, confer a health benefit on the host. Different strains have different effects.
- Considerations: Choose a reputable brand with multiple strains and a high CFU count (billions). Discuss with your doctor which strain might be best for your specific concerns (e.g., IBS, antibiotic-associated diarrhea).
- Timing: Some recommend taking probiotics on an empty stomach, others with food. Follow product instructions or doctor's advice.
- Prebiotics: Non-digestible food ingredients that selectively stimulate the growth and/or activity of beneficial bacteria in the colon. Think of them as food for your probiotics.
- Sources: Found naturally in many fiber-rich foods (garlic, onions, leeks, asparagus, bananas, oats, apples). Supplements often contain inulin or fructooligosaccharides (FOS).
- Caution: Can cause gas and bloating in some individuals, especially when first introduced. Start with small doses.
- Digestive Enzymes: These can help break down food, particularly for individuals with enzyme deficiencies or malabsorption issues. They can reduce the burden on the gut and alleviate symptoms like bloating.
- When to use: Often recommended for specific conditions like pancreatic insufficiency or after gallbladder removal. Not a universal solution for all gut problems.
- L-Glutamine: An amino acid that plays a role in gut barrier function and can be helpful for individuals with "leaky gut" or increased intestinal permeability.
Always consult your doctor or a registered dietitian before starting any new supplement regimen, especially if you have underlying health conditions or are taking other medications.
When to See a Doctor for Gut Concerns
While many gut issues can be managed with lifestyle and dietary changes, certain symptoms warrant immediate medical attention. Do not delay seeing a doctor if you experience:
- Severe or Persistent Abdominal Pain: Especially if it's new, worsening, or accompanied by other serious symptoms.
- Unexplained Weight Loss: Significant weight loss without trying can be a sign of an underlying serious condition.
- Blood in Stool or Black, Tarry Stools: This can indicate bleeding in the digestive tract and requires urgent evaluation.
- Persistent Diarrhea or Constipation: If changes in diet and lifestyle don't alleviate symptoms within a few weeks, or if symptoms are severe.
- Difficulty Swallowing (Dysphagia): This could indicate an obstruction or other serious issue.
- Persistent Nausea or Vomiting: Especially if accompanied by dehydration.
- Jaundice (Yellowing of Skin or Eyes): Can indicate liver or gallbladder problems.
- Family History of Digestive Diseases: If you have a family history of conditions like inflammatory bowel disease (Crohn's, ulcerative colitis) or colon cancer, be extra vigilant about symptoms.
Early diagnosis and intervention are crucial for many digestive conditions, so don't hesitate to seek professional medical advice.
Prevention: Maintaining a Healthy Gut for Life
The best approach to gut health is a proactive one. By consistently implementing healthy habits, you can support a thriving microbiome and prevent many common digestive issues.
- Embrace a Diverse, Plant-Rich Diet: Prioritize whole, unprocessed foods, focusing on a wide array of fruits, vegetables, legumes, and whole grains.
- Stay Hydrated: Drink plenty of water throughout the day.
- Manage Stress Effectively: Develop coping mechanisms for stress that work for you.
- Get Regular Physical Activity: Aim for a consistent exercise routine.
- Prioritize Quality Sleep: Make sleep a non-negotiable part of your health regimen.
- Limit Antibiotic Use: Use them only when necessary and under medical guidance.
- Avoid Smoking and Excessive Alcohol: Both are detrimental to gut health.
- Practice Good Hygiene: But don't be overly sterile; moderate exposure to diverse microbes from your environment (e.g., gardening, pets) can be beneficial.
Frequently Asked Questions (FAQs) About Gut Health
Is a 3-day juice cleanse good for my gut?
While a short juice cleanse might give your digestive system a temporary break from solid foods, it's unlikely to fundamentally "reset" your gut microbiome in a lasting way. Many juice cleanses lack sufficient fiber and protein, which are essential for feeding beneficial gut bacteria and maintaining overall health. They can also lead to nutrient deficiencies and blood sugar imbalances. A doctor would generally recommend a balanced, whole-food diet rich in fiber and fermented foods over restrictive juice cleanses for sustainable gut health.
How long does it take to improve gut health?
Significant and lasting improvements in gut health typically take weeks to months of consistent effort. While some dietary changes can induce shifts in the microbiome within days, truly rebalancing the ecosystem, increasing diversity, and healing the gut lining requires sustained commitment to a healthy diet and lifestyle. Think of it as a marathon, not a sprint.
What foods should I avoid for a healthy gut?
To promote a healthy gut, it's generally advisable to limit or avoid: processed foods high in sugar, unhealthy fats (trans fats, excessive saturated fats), and artificial ingredients; excessive red and processed meats; artificial sweeteners; and excessive alcohol. For some individuals, common allergens like gluten or dairy might also need to be reduced or avoided if they cause symptoms, but this should ideally be determined with professional guidance.
Are all probiotics the same?
No, all probiotics are not the same. Probiotic effects are strain-specific, meaning different strains of bacteria have different benefits. For example, Lactobacillus rhamnosus GG might be effective for antibiotic-associated diarrhea, while Bifidobacterium lactis DN-173 010 might help with constipation. It's important to choose a probiotic supplement that targets your specific health concerns and has been clinically studied for those benefits. Always consult your doctor or a pharmacist for guidance on choosing the right probiotic.
Can stress really affect my gut?
Absolutely. The gut and brain are intimately connected through the gut-brain axis. Stress can alter gut motility, increase intestinal permeability (leading to "leaky gut"), change the composition of the gut microbiome, and exacerbate symptoms of digestive disorders like IBS. Managing stress through techniques like mindfulness, meditation, yoga, and regular exercise is a crucial component of maintaining good gut health.
Conclusion
The idea of a "3-day gut reset" is appealing, but the reality is that truly nurturing your gut health requires a more sustained and holistic approach. While short-term dietary adjustments can initiate changes, lasting improvements in your gut microbiome and overall digestive well-being stem from consistent, evidence-based practices. A doctor's perspective emphasizes a diverse, plant-rich diet, regular exercise, effective stress management, adequate sleep, and judicious use of antibiotics. If you're experiencing persistent gut symptoms, don't hesitate to consult a healthcare professional for personalized advice and diagnosis. By committing to these foundational principles, you can cultivate a resilient gut that supports your health for years to come, far beyond the promise of a fleeting three-day fix.
Sources / Medical References
- Singh, R. K., et al. (2017). Influence of diet on the gut microbiome and implications for human health. Journal of Translational Medicine, 15(1), 73.
- Marchesi, J. R., et al. (2016). The gut microbiota and host health: a new frontier for translational medicine. Gut, 65(2), 330-339.
- Cryan, J. F., & Dinan, T. G. (2012). Mind-altering microorganisms: the impact of the gut microbiota on brain and behaviour. Nature Reviews Neuroscience, 13(10), 701-712.
- Hills, R. D., et al. (2019). Gut Microbiome: Profound Implications for Diet and Disease. Nutrients, 11(7), 1613.
- Harvard Health Publishing. (2021). The gut-brain connection. Retrieved from https://www.health.harvard.edu/diseases-and-conditions/the-gut-brain-connection
- Mayo Clinic. (2022). Probiotics: What you need to know. Retrieved from https://www.mayoclinic.org/diseases-conditions/digestive-system-diseases/in-depth/probiotics/art-20046517
- Healthline. (2023). Reset Your Gut in 3 Days? Doctor Explains What Actually Works. Retrieved from https://www.healthline.com/health/video/reset-your-gut-in-3-days-doctor-explains-what-actually-works