Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand what constitutes a low vitamin D level, its common symptoms, causes, and effective treatments. Learn how to maintain optimal vitamin D for bone health, immune function, and overall well-being. Discover when to seek medical advice for vitamin D deficiency.

Pre- and post-workout nutrition are two of the most impactful yet frequently confused aspects of sports nutrition. The right foods at the right times can meaningfully improve performance, accelerate recovery, and maximise muscle adaptation — here's exactly what to eat and when.
April 14, 2026
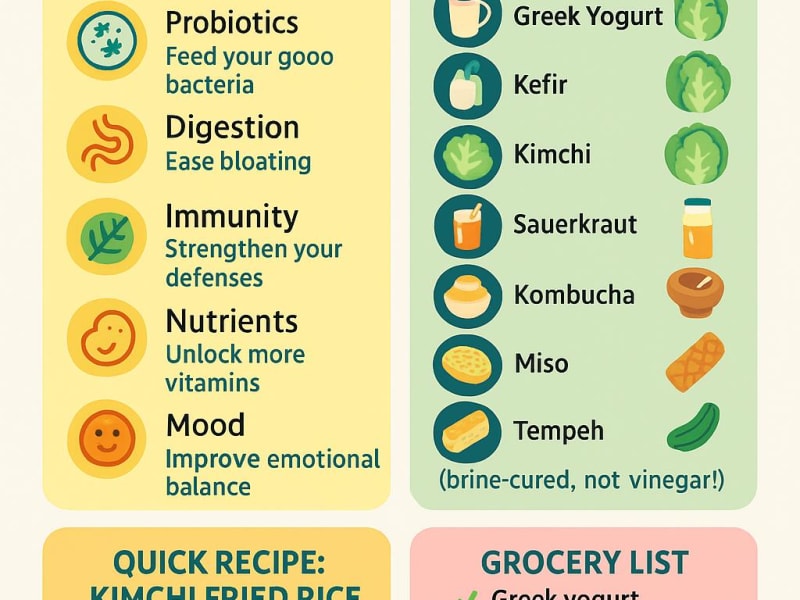
Fermented foods have nourished human gut health for millennia — and modern science is now confirming the mechanisms behind their benefits. From kefir to kimchi, this beginner's guide explains what fermented foods do in the body and how to incorporate them confidently.
April 14, 2026


Vitamin D, often dubbed the 'sunshine vitamin,' is much more than just a nutrient; it's a crucial hormone that plays a pivotal role in nearly every bodily function. From strengthening your bones to bolstering your immune system, its influence is widespread and profound. Yet, despite its importance, vitamin D deficiency is a global health concern, affecting a significant portion of the population across all age groups.
Understanding what constitutes a 'low' vitamin D level is the first step toward safeguarding your health. This comprehensive guide will delve into the definitions of deficiency and insufficiency, explore the myriad symptoms associated with low levels, uncover common causes, explain diagnostic methods, and outline effective treatment and prevention strategies. By the end, you'll have a clearer picture of your vitamin D needs and when it's time to consult a healthcare professional.
Vitamin D is a fat-soluble vitamin that is unique because our bodies can produce it when exposed to sunlight. It primarily exists in two forms:
Once produced or ingested, vitamin D undergoes a series of conversions in the liver and kidneys to become its active form, 1,25-dihydroxyvitamin D, also known as calcitriol. This active form is what performs vitamin D's essential functions throughout the body.
The role of vitamin D extends far beyond just bone health. Its active form acts like a hormone, influencing numerous physiological processes:
Perhaps its most well-known function, vitamin D is critical for calcium and phosphate absorption in the gut. These minerals are essential for building and maintaining strong bones. Without adequate vitamin D, bones can become thin, brittle, or misshapen, leading to conditions like rickets in children and osteomalacia (soft bones) and osteoporosis (porous bones) in adults.
Vitamin D modulates both innate and adaptive immune responses. Adequate levels are associated with a reduced risk of infections, including respiratory tract infections, and may play a role in reducing the risk of autoimmune diseases.
Receptors for vitamin D are found in muscle tissue, and low levels have been linked to muscle weakness, particularly in older adults, increasing the risk of falls.
Some research suggests a link between vitamin D deficiency and mood disorders, including depression. While more studies are needed, maintaining sufficient levels may contribute to overall mental well-being.
Emerging research indicates that vitamin D may play a role in cardiovascular health by influencing blood pressure regulation and reducing inflammation, though its direct impact on heart disease prevention is still being investigated.
Studies are ongoing to explore vitamin D's potential involvement in reducing the risk of certain cancers, type 2 diabetes, and other chronic diseases.
Vitamin D levels are measured by a blood test that checks the amount of 25-hydroxyvitamin D (25(OH)D) in your blood. This is the main circulating form of vitamin D, and its levels accurately reflect your body's stores.
While there's still some debate among medical organizations regarding the precise optimal ranges, a general consensus exists for defining deficiency and insufficiency:
Note: Some organizations, like the Endocrine Society, recommend even higher optimal levels, often suggesting 40-60 ng/mL for general health and up to 100 ng/mL for specific conditions or populations. Always discuss your specific levels and goals with your doctor.
Many people with low vitamin D levels experience no noticeable symptoms, especially in the early stages of insufficiency. However, as levels drop further into deficiency, or if they remain low for extended periods, a range of symptoms can emerge. These can be subtle and often mistaken for other conditions, making diagnosis challenging without a blood test.
It's important to remember that these symptoms can also be indicative of other health problems. Therefore, self-diagnosis is not recommended. If you experience any of these symptoms persistently, it's crucial to consult a healthcare professional.
Several factors can contribute to low vitamin D levels, ranging from lifestyle choices to underlying medical conditions:
This is the most common cause globally. Factors include:
Few foods naturally contain significant amounts of vitamin D. Rich sources include:
Strict vegan or vegetarian diets can be particularly low in vitamin D unless fortified foods or supplements are regularly consumed.
Conditions that impair fat absorption in the gut can lead to vitamin D deficiency, as it is a fat-soluble vitamin. These include:
The liver and kidneys are essential for converting vitamin D into its active form. Chronic diseases affecting these organs can impair this conversion, leading to deficiency.
Body fat can sequester vitamin D, meaning more vitamin D is needed for obese individuals to achieve sufficient blood levels. The vitamin D gets trapped in fat cells, making it less available for use by the body.
Some medications can interfere with vitamin D metabolism or absorption, including:
As people age, their skin becomes less efficient at producing vitamin D from sunlight, and their kidneys may be less effective at converting it to its active form. Older adults also tend to spend more time indoors.
Individuals with darker skin tones have higher amounts of melanin, a pigment that reduces the skin's ability to produce vitamin D from sun exposure. They may require significantly more sun exposure than those with lighter skin to produce the same amount of vitamin D.
The only reliable way to diagnose vitamin D deficiency or insufficiency is through a blood test. Your doctor will typically order a test for:
While routine screening for everyone is not always recommended, certain individuals should consider getting their vitamin D levels checked:
Discuss with your doctor if a vitamin D test is appropriate for you.
Treatment for low vitamin D levels typically involves increasing intake through diet, sun exposure, and most commonly, supplementation. The specific approach and dosage will depend on the severity of the deficiency, individual risk factors, and your doctor's recommendations.
While sun exposure is the primary natural source of vitamin D, it must be approached cautiously to avoid skin damage and cancer risk.
Incorporating more vitamin D-rich foods into your diet can help maintain levels, but it's often not enough to correct a deficiency on its own.
For most individuals with vitamin D deficiency, supplements are the most effective and reliable way to raise blood levels. Vitamin D3 (cholecalciferol) is generally preferred over D2 due to its greater efficacy in raising and maintaining vitamin D levels.
After starting treatment, your doctor will likely recommend retesting your 25(OH)D levels after a few months (typically 2-3 months) to ensure that your levels are improving and to adjust the dosage as needed. Once optimal levels are achieved, a maintenance dose is usually recommended.
Prevention is always better than cure. Here are strategies to maintain healthy vitamin D levels:
It's advisable to consult a doctor if:
A simple blood test can confirm your vitamin D status, and your doctor can provide personalized recommendations for treatment and prevention.
A: Yes, it is possible to get too much vitamin D, but it's very rare from sun exposure or diet alone. Vitamin D toxicity (hypervitaminosis D) almost always occurs from excessive supplementation, especially with very high doses taken over a long period without medical supervision. Symptoms of toxicity include nausea, vomiting, poor appetite, constipation, weakness, and kidney problems due to high calcium levels in the blood.
A: The time it takes to correct a deficiency depends on the initial level of deficiency, the dosage of supplementation, and individual factors. Typically, with appropriate high-dose supplementation under medical guidance, it can take several weeks to a few months (2-3 months) to bring blood levels into the sufficient range. Maintenance therapy is then usually required.
A: Vitamin D2 (ergocalciferol) is plant-derived, while Vitamin D3 (cholecalciferol) is animal-derived and also produced in the skin from sun exposure. Studies generally show that Vitamin D3 is more effective at raising and maintaining blood levels of 25(OH)D compared to D2, making D3 the preferred form for supplementation.
A: For many people, especially those living at higher latitudes, with darker skin, or who spend most of their time indoors, sun exposure alone is often not enough to maintain optimal vitamin D levels year-round. Factors like season, time of day, cloud cover, sunscreen use, and skin pigmentation all affect vitamin D production from the sun. Dietary intake and supplementation are often necessary.
A: Yes, vitamin D supplements can interact with certain medications. For example, they can affect the absorption of certain cholesterol-lowering drugs (bile acid sequestrants), weight-loss drugs (Orlistat), and corticosteroids. High doses of vitamin D can also interact with digoxin (for heart conditions) and diuretics. Always inform your doctor about all supplements and medications you are taking.
Vitamin D is an indispensable nutrient vital for a multitude of bodily functions, extending beyond bone health to immune regulation, mood, and muscle strength. Understanding what constitutes a low vitamin D level—typically below 20 ng/mL for deficiency and 20-29 ng/mL for insufficiency—is crucial for proactive health management. While symptoms like fatigue, bone pain, and frequent infections can indicate a problem, often the deficiency is silent, making regular monitoring for at-risk individuals essential.
Factors like limited sun exposure, dietary habits, certain medical conditions, and even skin pigmentation can contribute to low levels. Fortunately, deficiency is highly treatable through controlled sun exposure, dietary adjustments, and most effectively, vitamin D3 supplementation under medical guidance. By taking proactive steps and consulting with your healthcare provider, you can ensure your vitamin D levels are optimized, paving the way for better overall health and well-being.
This article is based on general medical consensus and guidelines from reputable health organizations, including but not limited to:
For personalized medical advice, always consult with your healthcare provider.
Plant proteins vary significantly in amino acid completeness and digestibility — and choosing the right ones matters for muscle maintenance, satiety, and overall health. This ranked guide separates the best plant protein sources from those that need strategic pairing.
April 14, 2026