Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Pneumonia poses a greater risk to older adults, often presenting with atypical symptoms. Learn about the signs, causes, diagnosis, treatment, and prevention strategies to protect seniors' health.
Uncover the cause of digestive issues with a stool wet mount test. Learn how this simple diagnostic tool detects parasites, when it's needed, and how to prepare.
April 20, 2026
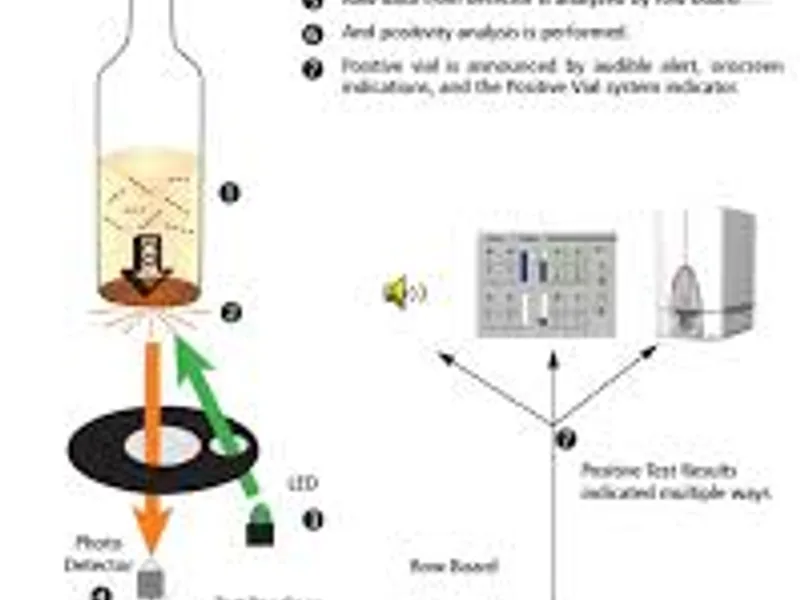
Discover how automated blood cultures for fungus offer rapid, reliable results, improving patient care and treatment outcomes in India.
April 20, 2026
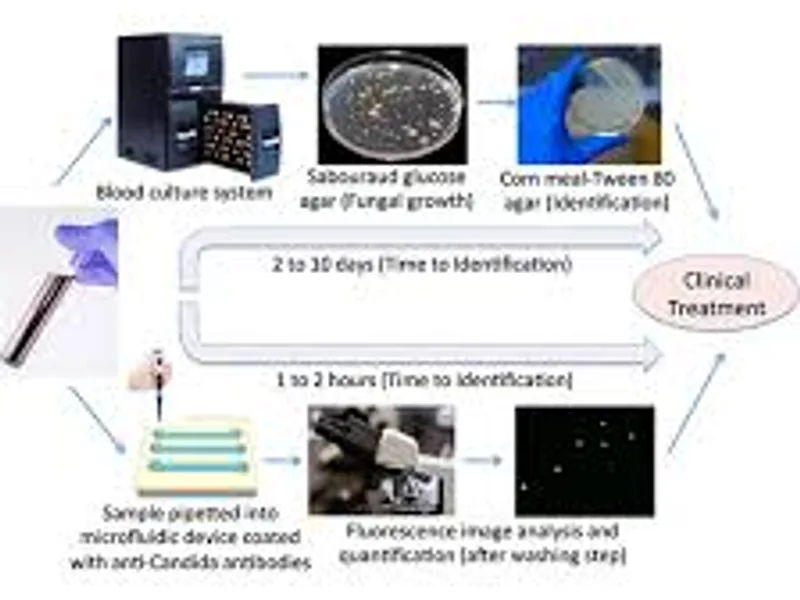
Discover how automated paired blood cultures revolutionize fungemia diagnosis. This advanced test offers faster, more accurate results for critical fungal infections.
April 20, 2026

Pneumonia, an infection that inflames the tiny air sacs in your lungs (alveoli), can be a serious concern, especially for older adults. While anyone can develop pneumonia, those aged 65 and above face a higher risk of severe illness, hospitalization, and even mortality. In fact, estimates suggest that nearly 1 million adults over 65 are hospitalized with pneumonia annually in the United States alone, making it a significant health challenge for this age group.
The challenge with pneumonia in older adults lies not only in its increased severity but also in its often atypical presentation. Symptoms can be more subtle, easily missed, or masked by existing chronic conditions. This can lead to delayed diagnosis and treatment, potentially worsening outcomes. Recognizing these nuances is key for timely intervention and effective management.
Several factors contribute to the increased vulnerability of older adults to pneumonia:
While some symptoms of pneumonia are common across all age groups, older adults may experience them differently or present with a unique set of signs. It's important to be aware of these variations:
Even with atypical presentations, older adults can still experience classic pneumonia symptoms, which may include:
Consider this scenario: Mrs. Sharma, an 80-year-old woman living independently, suddenly starts refusing meals and seems unusually lethargic. Her daughter notices she's also a bit unsteady when walking. While she doesn't have a fever or a cough, her daughter feels something is wrong and calls the doctor. Mrs. Sharma is later diagnosed with pneumonia.
Pneumonia can be caused by various microorganisms. The specific cause often determines the type of pneumonia. In older adults, the most common culprits include:
This is the most common type. Streptococcus pneumoniae (pneumococcus) is a frequent cause. Other bacteria like Haemophilus influenzae and Mycoplasma pneumoniae can also cause it.
Viruses are also significant causes, especially in older adults. These include viruses responsible for:
Viral pneumonia can sometimes lead to secondary bacterial infections, complicating the illness.
This type is acquired in healthcare settings like hospitals or long-term care facilities. Older adults who are hospitalized or reside in these facilities are at higher risk due to exposure to different, often more resistant, bacteria.
This occurs when foreign substances, such as food, liquids, saliva, or vomit, are inhaled into the lungs. It's more common in individuals with swallowing difficulties (dysphagia), which can be related to age, stroke, or neurological conditions.
Accurate diagnosis is vital for effective treatment. Doctors typically use a combination of methods:
Treatment aims to clear the infection, manage symptoms, and prevent complications. The approach depends on the cause, severity, and the individual's overall health:
Prevention is always better than cure. Several measures can significantly reduce the risk of developing pneumonia:
Prompt medical attention is essential if you or an older adult you care for experiences symptoms suggestive of pneumonia. Don't delay seeking help, especially if:
Early diagnosis and treatment can make a significant difference in recovery and prevent serious complications.
Yes, with appropriate medical treatment, most cases of pneumonia in older adults can be cured. However, the recovery period might be longer compared to younger individuals, and there's a risk of recurrence, especially if underlying health issues aren't well-managed.
Pneumonia itself can be caused by germs that are contagious, like bacteria and viruses. However, the severity and how it spreads can vary. Good hygiene and vaccination are key preventive measures.
While age itself is a risk factor due to a naturally weaker immune system, having underlying chronic health conditions like COPD, heart disease, or diabetes significantly increases the risk and potential severity of pneumonia.