Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Learn about the Aspergillus precipitin test, a blood test used to detect antibodies against the Aspergillus fungus. Understand its purpose, how it's performed, and what the results mean for diagnosing and managing fungal infections like aspergillosis.

Have you ever heard of the Aspergillus precipitin test? It might sound technical, but understanding it can be incredibly helpful if your doctor suspects a fungal infection caused by Aspergillus . This common fungus is found everywhere, from your home to outdoor spaces like decaying leaves and compost piles. While most of us breathe in Aspergillus spores daily without any issues, some individuals, particularly those with weakened immune systems, can develop serious health problems. This blog post will break down what the Aspergillus precipitin test is, why it's done, what the results mean, and how it helps in diagnosing and managing aspergillosis, a group of infections caused by this fungus. What is Aspergillosis? Aspergillosis refers to a range of illnesses caused by Aspergillus fungi. These fungi are widespread, thriving in environments like decaying organic matter and even on certain plants. The spores are constantly in the air, and most people inhale them without consequence. However, for individuals with compromised immune systems – such as those living with HIV, undergoing chemotherapy, or taking immunosuppressant drugs after an organ transplant – these spores can lead to significant infections. There are primarily two types of aspergillosis that can affect people: Allergic Bronchopulmonary Aspergillosis (ABPA): This condition triggers allergic reactions, leading to symptoms like wheezing and coughing. It's particularly common in people who already have conditions like asthma or cystic fibrosis. In fact, ABPA affects a notable percentage, up to 19 percent, of individuals with cystic fibrosis. Invasive Aspergillosis: This is a more severe form where the infection can spread from the lungs throughout the body via the bloodstream. It poses a significant risk to vital organs, including the lungs, kidneys, heart, brain, and nervous system, especially in those with weakened immunity. Common Symptoms of Aspergillosis The signs of aspergillosis can vary greatly from person to person. Some might experience a simple dry cough, while others could cough up significant amounts of blood, which is a medical emergency requiring immediate attention. Generally, symptoms can include: A general feeling of unwellness Fatigue and weakness Unexplained weight loss Fever (often high and persistent) Coughing, which might be dry or produce phlegm (sputum) Shortness of breath Chest pain Coughing up blood (hemoptysis) For individuals with underlying conditions like asthma or cystic fibrosis, the symptoms of aspergillosis can be particularly severe. They might notice a significant worsening of their existing symptoms, such as: Increased production of phlegm Worsening asthma symptoms, especially with physical activity More frequent or severe wheezing A persistent cough that doesn't improve Real-life scenario: Imagine Mrs. Sharma, who has had asthma for years. Recently, her cough has become much worse, she's feeling unusually tired, and her chest feels tight even when she's resting. Her doctor, noticing these changes and her existing condition, might consider aspergillosis and order further tests. Understanding the Aspergillus Precipitin Test The Aspergillus precipitin test is a diagnostic tool your doctor might use. It works by detecting and measuring specific antibodies in your blood that your immune system creates in response to Aspergillus . Think of antibodies as specialized soldiers your body produces to fight off invaders, called antigens. Aspergillus , or its components, can act as an antigen. There are different types of antibodies, known as immunoglobulins. The precipitin test commonly looks for three types: IgM (Immunoglobulin M): Typically indicates a recent or current infection. IgG (Immunoglobulin G): Suggests a past exposure or current infection, as these antibodies can remain in the system for a long time. IgE (Immunoglobulin E): Often associated with allergic reactions, making it particularly relevant for diagnosing conditions like ABPA. By identifying the presence and levels of these antibodies, the test helps doctors determine if Aspergillus is present and how your body is reacting to it. How the Test is Performed The procedure for an Aspergillus precipitin test is straightforward and involves a simple blood draw. Your doctor will provide specific instructions, which might include fasting for a certain period before the test, though this isn't always necessary. Here’s what you can expect: Preparation: The healthcare provider will identify a suitable vein, usually in the bend of your elbow. Cleaning: The skin at the collection site will be cleaned thoroughly with an antiseptic to prevent infection. Blood Draw: A sterile needle will be inserted into the vein to collect a blood sample. An elastic band might be placed around your arm to make the veins more prominent. Post-procedure: Once the sample is collected, the needle is removed, and a small bandage is applied. If there's any minor bleeding after the needle is removed, applying gentle pressure with three fingers for a couple of minutes can help stop it and minimize bruising. The collected blood sample is then sent to a laboratory for analysis. The results are usually available within one to two days. Interpreting Your Test Results Interpreting the results of an Aspergillus precipitin test requires a doctor's expertise, as they consider these findings alongside your symptoms, medical history, and other diagnostic information. Positive Result: A positive result means that specific antibodies against Aspergillus were detected in your blood. This strongly suggests exposure to the fungus and potentially an active infection or an allergic reaction. The type and level of antibodies found (IgM, IgG, IgE) help differentiate between acute, chronic, or allergic forms of aspergillosis. Negative Result: A negative result typically indicates that no significant levels of these antibodies were found. While this often rules out aspergillosis, in some rare cases, especially in individuals with severely compromised immune systems, the body might not produce enough antibodies for detection. Therefore, your doctor might still consider other diagnostic methods if suspicion remains high. Treatment Approaches for Aspergillosis Treatment for aspergillosis depends heavily on the type and severity of the infection, as well as the patient's overall health, particularly their immune status. The primary goal is to clear the fungal infection and manage any associated symptoms or complications. Antifungal Medications: These are the cornerstone of treatment. For invasive aspergillosis or severe infections, potent antifungal drugs like voriconazole or isavuconazole are often prescribed. For less severe cases or ABPA, other antifungals like itraconazole might be used. People with weakened immune systems may require prolonged treatment, sometimes lasting for several months to even years, to effectively eradicate the fungus. Allergy Management: For ABPA, treatment focuses on reducing the allergic reaction to the fungus. This can involve antifungal medications to lower the fungal load, alongside corticosteroids to control inflammation and allergy symptoms. Antihistamines might also be recommended. Supportive Care: This includes managing symptoms like shortness of breath, pain, and fatigue. For severe lung infections, oxygen therapy might be necessary. Good nutrition and rest are also vital components of recovery. Surgical Intervention: In rare, severe cases, such as the formation of fungal balls (aspergillomas) or localized abscesses, surgery might be considered to remove the infected tissue. Preventing Aspergillus Exposure While completely avoiding Aspergillus spores is impossible due to their widespread presence, certain measures can help reduce exposure, especially for those at higher risk: Minimize Exposure to Dust and Mold: Regularly clean your home, especially areas prone to dampness or mold growth. Use exhaust fans in bathrooms and kitchens. Avoid activities that stir up dust, such as gardening in dry conditions or visiting construction sites, if you are particularly vulnerable. Maintain a Strong Immune System: For individuals with weakened immunity, following medical advice regarding treatment, nutrition, and hygiene is paramount. Ensure vaccinations are up-to-date as recommended by your doctor. Be Cautious in Certain Environments: If you have a compromised immune system, it might be advisable to avoid environments with high concentrations of mold or dust, such as compost heaps, poorly ventilated buildings, or areas with significant water damage. When to Consult a Doctor It's important to seek medical advice if you experience symptoms that could indicate aspergillosis, especially if you have risk factors like a weakened immune system, asthma, or cystic fibrosis. Pay close attention to: Sudden worsening of respiratory symptoms (cough, shortness of breath, wheezing). Fever that doesn't resolve with usual treatments. Coughing up blood or significant amounts of discolored phlegm. Unexplained fatigue or feeling generally unwell. Your doctor can assess your symptoms, medical history, and recommend the appropriate diagnostic tests, including the Aspergillus precipitin test, to determine the cause and initiate timely treatment. Frequently Asked Questions (FAQ) Q1: How long does it take to get Aspergillus precipitin test results? Typically, the results for an Aspergillus precipitin test are available within 1 to 2 days after the blood sample is sent to the laboratory. Q2: Can you have aspergillosis without a positive precipitin test? While a positive test is a strong indicator, it's possible, though less common, to have aspergillosis with a negative precipitin test, especially in individuals with severely weakened immune systems who may not produce detectable antibody levels. Your doctor will consider all clinical information when making a diagnosis. Q3: Is aspergillosis contagious? Aspergillosis is not typically spread from person to person. It is caused by inhaling spores of the Aspergillus fungus, which are present in the environment. Q4: What is the
In summary, timely diagnosis, evidence-based treatment, and prevention-focused care improve long-term health outcomes.
Uncover the cause of digestive issues with a stool wet mount test. Learn how this simple diagnostic tool detects parasites, when it's needed, and how to prepare.
April 20, 2026
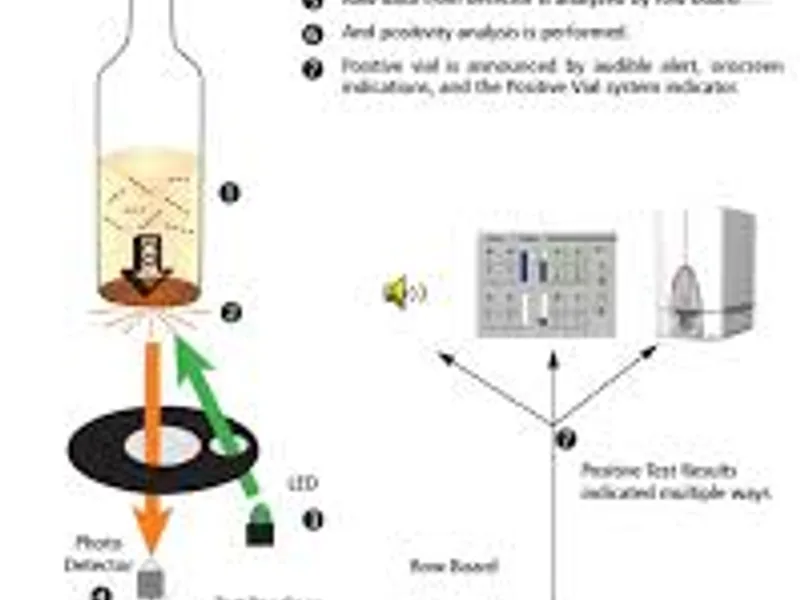
Discover how automated blood cultures for fungus offer rapid, reliable results, improving patient care and treatment outcomes in India.
April 20, 2026
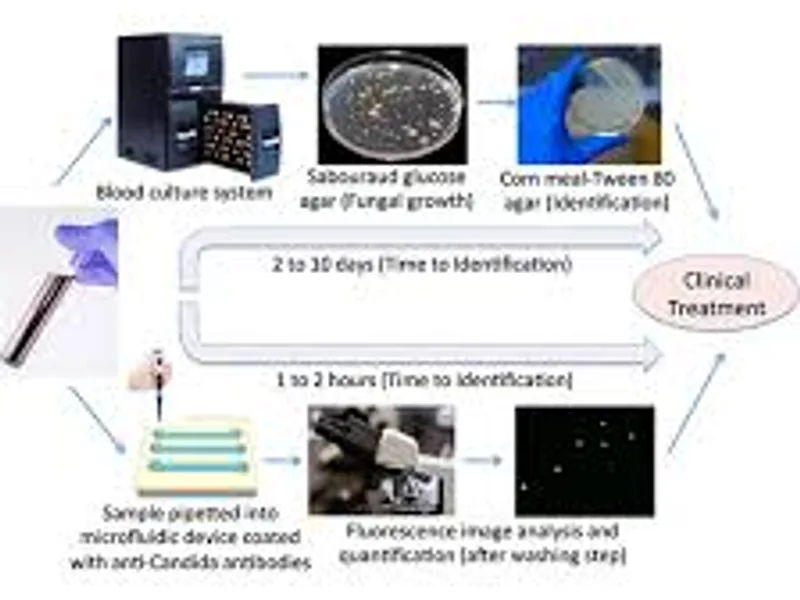
Discover how automated paired blood cultures revolutionize fungemia diagnosis. This advanced test offers faster, more accurate results for critical fungal infections.
April 20, 2026